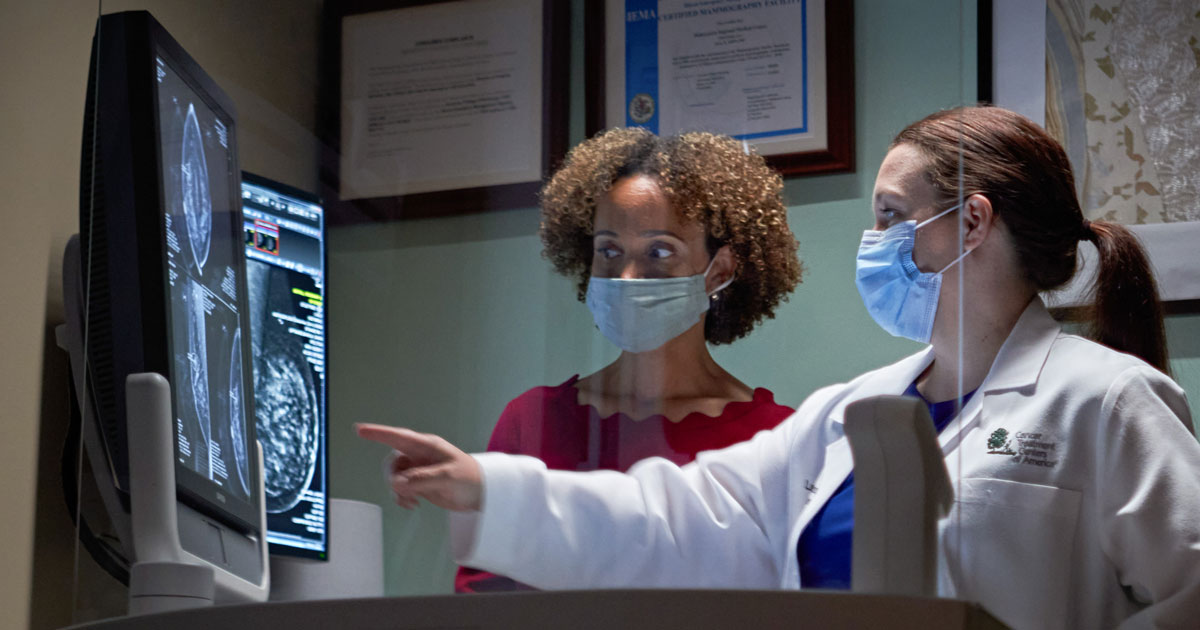
Getting screened for breast cancer is a regular routine for many American women. According to the Susan G. Komen Foundation, 75 percent of women 50 to 74 years old with health insurance have had a mammogram in the last two years.
But the numbers are dramatically lower for the uninsured, minorities and gay and bisexual women, who are much less likely to get screened for breast cancer. That means they have a higher chance of missed or advanced-stage diagnoses, since breast cancer patients who had been screened more regularly were more likely to get diagnosed at an early stage, when treatments may produce more positive outcomes.
Nearly 100 percent of women whose breast cancer is found early survive at least five years, making screening tests a valuable tool in early detection. Thanks in part to these screening tools, fewer women are dying from breast cancer today than a decade ago.
Screening tests are routine exams recommended for women based on a variety of factors, including family history and age, and performed on a regular basis and in the absence of sign or symptoms.
This article will explore:
- Who should be screened for breast cancer?
- Screening setbacks during the pandemic
- What are the signs and symptoms of breast cancer?
- What is a mammogram?
- How to prepare for a mammogram
- What to expect during your mammogram
- How long does it take to get mammogram results?
- Other ways to screen for breast cancer
- Breast Cancer Centers and programs at Cancer Treatments Centers of America® (CTCA) and City of Hope®
If you're interested in scheduling a cancer screening with us, or if you believe you have symptoms of cancer and want to schedule an appointment for a diagnostic evaluation, call us or chat online with a member of our team.
Who should be screened for breast cancer?
Whether and how often you get screened for breast cancer depends on your age as well as your personal and family medical history. For the average woman, research has shown the chance of developing breast cancer is significantly reduced if she begins yearly breast cancer screenings with a mammogram at age 40. Depending on their risk factors, some women may start screening at a younger age and have tests more frequently as they age.
The American Cancer Society (ACS), the American College of Radiology (ACR) and the Society of Breast Imaging recommend women at average risk for developing breast cancer begin annual screening mammograms between ages 40 and 44. Women 45 to 54 years old should get mammograms each year, while those age 55 and older should be screened every other year, as long as they’re in good health and have a life expectancy of at least 10 years.
Women at higher risk of breast cancer include those who:
- Have a close relative, such as a parent, sibling, child, aunt or cousin diagnosed with breast cancer
- Had genetic testing that revealed they or a close relative carries the BRCA1 or BRCA2 gene mutation
- Had radiation therapy to the chest between age 10 and 30
- Have a family history of Li-Fraumeni syndrome, Cowden syndrome, or Bannayan-Riley-Ruvalcaba syndrome
If you think your family history puts you at higher risk, the American Society of Breast Surgeons recommends women receive a breast cancer risk assessment around age 25. Generally, women in the high-risk category begin screening tests at age 30.
Screening is particularly important for anyone with any type of previous cancer diagnosis.
“I think a lot of patients are so focused on surviving, on getting through their chemotherapy, their surgery and so forth, that they forget about picking up the pieces and screening for other cancers,” says Brittany Bradford, MSN, NP, City of Hope Survivorship Program Nurse Practitioner, who spearheaded the new screening program.
Screening setbacks during the pandemic
Research published in The Journal of the American Medical Association found that through 2020, the first year of the COVID-19 pandemic, breast cancer screenings declined by 6 percent. A 2022 study by the ACR found pre-pandemic breast cancer screenings are still not back to pre-pandemic levels.
“A major concern is that cancer diagnoses dropped by nearly 50 percent in the peak-pandemic period and have not rebounded completely to the pre-COVID rate,” said study author Lars J. Grimm, MD, associate professor at Duke University Medical Center. “This could lead to a rise in future cancer diagnoses and a larger proportion of later-stage diagnoses with associated worse prognoses.”
What are the signs and symptoms of breast cancer?
After skin cancer, breast cancer is the most common type of cancer in American women. It’s more likely to occur as women age and is more prevalent in black women.
Being aware of any changes in your breasts is important. Women should be vigilant for possible signs and symptoms of breast cancer, such as:
- Unusual breast swelling or pain
- A lump in the breast, under the arm or on the collarbone
- Skin dimpling on the breast
- Inverted nipple
- Nipple discharge
But remember, regular breast screenings are intended to detect possible signs of the disease before symptoms develop.
What is a mammogram?
Mammography is the most common and widely used breast cancer screening tool.
A mammogram is a low-dose X-ray of the breast designed to detect cancers too small to be felt in a manual examination or to cause symptoms. According to the National Institutes of Health, only about one in five cancers are missed by a mammogram.
Mammography has been around since the 1970s, and the technology has advanced over the years, with digital imaging introduced in the early 2000s and digital breast tomosynthesis (DBT), also known as 3D mammography, available more recently.
DBT provides very detailed views of breast tissue and is particularly helpful in women with dense breast tissue.
How to prepare for a mammogram
Mammograms are performed by specially trained technicians in a private room at a hospital or imaging facility. These tests capture images that are read and interpreted by a radiologist, a physician trained to identify suspicious signs that may need follow-up testing.
Keep these tips in mind as you prepare for your mammogram:
- If you haven’t started menopause, try to schedule your mammogram when your breasts are not tender due to your menstrual cycle, usually about a week after your period.
- Bring your doctor’s name and contact information so your test results can be sent to him or her.
- Don’t wear deodorant, antiperspirant, perfumes, powders or lotions on your upper body the day of the screening, since these products may interfere with the imaging.
- You’ll be asked to remove clothing from your upper body and to wear a short gown, so wear a shirt and pants or skirt rather than a dress so your lower body remains covered.
What to expect during your mammogram
During a mammogram, each breast is placed on a clear plastic plate and compressed between that and another plate to flatten the breast and hold it still while the X-ray is taken. The compression lasts about 10 to 15 seconds and may be uncomfortable or painful.
The technician likely will take two images of each breast—one from the top and one from the side. The procedure from check-in until the time you leave usually takes about 30 minutes.
How long does it take to get mammogram results?
Doctors will examine the results of your test and score it using the Breast Imaging Reporting and Data System or BI-RADS categories, which range from one (not cancer) to six (high likelihood of cancer). A category 0 means more tests are needed. Mammogram reports also rank breast density from A (not dense) to D (very dense.)
The results of your mammogram will be sent to you and your doctor, usually within 10 days. If the radiologist needs more information to identify an irregularity in the images, he or she may order a follow-up mammogram, ultrasound or MRI.
Undergoing regular mammograms is helpful since they allow comparisons over time to identify changes or abnormalities unique to your breasts.
Other ways to screen for breast cancer
The goal of any screening test is to detect abnormalities early—before you’re aware they exist. Screening tests for breast cancer include:
- Self-exams
- Ultrasound
- MRI
Self-exams
The ACS no longer recommends breast self-examinations for anyone at average risk of breast cancer. This change in recommendations evolved after studies found that self-exams didn’t provide enough of a benefit for early detection and may also lead to unnecessary biopsies. That doesn’t mean you should never do a self-exam. But understand that they aren’t as effective as other screening methods, especially mammograms.
Ultrasound
Breast ultrasound, which uses soundwaves to create computer images of breast tissue, is able to detect fluid-filled cysts, which may not be easy to identify on a mammogram. Ultrasound is generally not used for routine screening but instead as a follow-up to a mammogram.
Magnetic resonance imaging (MRI)
MRI uses a magnet, radio waves and imaging software to produce detailed images of the breast. MRI is not usually used as a breast cancer screening tool but as a follow-up to a mammogram or for women with a high-risk profile.

Breast cancer screening and care at CTCA and City of Hope
Breast cancer is the second-most diagnosed cancer among women in the United States, affecting one in eight women who live to the age of 80. The disease is expected to account for 287,850 new cancer cases in 2022, according to the ACS, and 7 percent of all cancer deaths each year. At CTCA and City of Hope, our breast cancer experts work on a multidisciplinary team at dedicated breast cancer centers and programs designed not only to treat breast cancer, but to identify high-risk patients and offer cancer guidance for screenings and prevention.
CTCA High-Risk Breast Cancer Programs
The High-Risk Breast Cancer Programs at CTCA Atlanta, CTCA Chicago and CTCA Phoenix offer services for women who know they’re at risk for breast cancer or who may be concerned about their likelihood of developing the disease.
The multidisciplinary team of cancer experts, genetic counselors and supportive care providers at CTCA will work with you to determine the level of your risk and empower you to take control.
CTCA Breast Cancer Centers
The Breast Cancer Centers at CTCA Atlanta, CTCA Chicago and CTCA Phoenix each bring together expert teams of doctors and clinicians who focus specifically on breast cancer. The experts at the Breast Cancer Centers at CTCA have the experience to help you navigate the complexities of choosing a treatment plan tailored to your needs. If a mammogram or other screening test shows an abnormality, our experts have years of advanced training and the expertise treating a wide variety of breast cancer types, including triple-negative breast cancer and inflammatory breast cancer.
The Breast Cancer Centers also are involved in clinical trials for precision treatments and innovative technologies, including targeted therapy. These trials may offer participants options that may have otherwise been unavailable to them.
Breast Cancer Program at City of Hope
CTCA is now part of City of Hope, one of the nation’s top 10 cancer hospitals and a National Cancer Institute-designated comprehensive cancer center. CTCA and City of Hope are committed to working together to broaden access to high-quality and compassionate care for patients with breast or other cancers. City of Hope is recognized for the quality of its breast cancer care and for advancing the field of breast cancer through groundbreaking, evidence-based research, on-site innovative clinical trials, leading-edge treatment and premier patient care. At City of Hope, breast cancer clinicians and researchers collaborate extensively to develop and evaluate new therapies intended to improve survival and quality-of-life outcomes.
The services at the City of Hope Breast Cancer Program include:
- Early detection, screening and prevention resources
- Breast cancer risk assessment based on genetics, lifestyle and environmental factors
- Advanced treatments, including state-of-the art surgical techniques, high-precision radiation therapy and immunotherapy
- Survivorship and follow-up program focused on reducing the risk of recurrence and improving quality of life


