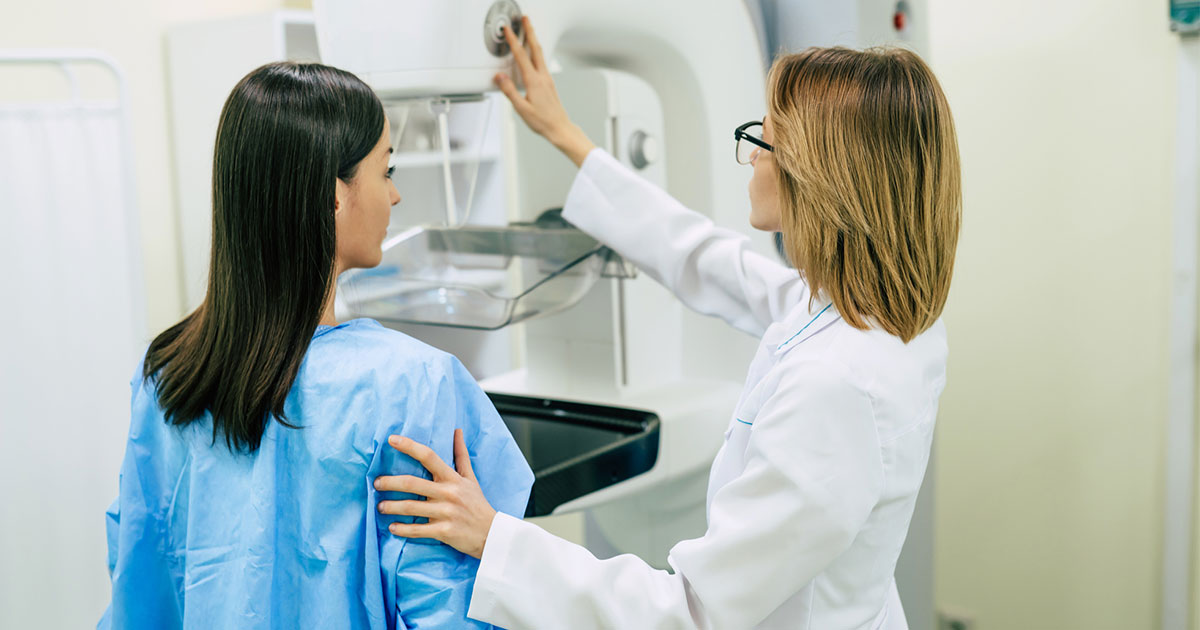
Regularly scheduled mammograms, combined with improved breast cancer detection technology, have led to a steady drop in mortality rates for women diagnosed with this disease.
In fact, today, fewer women are dying from breast cancer than 10 years ago. The improvement in survival rate is due, in part, to better cancer-fighting drugs and improved surgical techniques and technology. The biggest factor, though, is that doctors are finding breast cancer earlier, frequently before the cancer has had a chance to spread to nearby lymph nodes or other parts of the body. The key to those early detections: mammography.
Mammograms themselves have changed over the years, giving doctors a much clearer look at abnormal developments in a breast and a better understanding of when additional tests are warranted. The development of a 3D-like mammogram, called digital breast tomosynthesis (DBT), has been a major advancement for cancer detection.
As a Radiologist at Cancer Treatment Centers of America® (CTCA) who specializes in women’s imaging services, I’ve seen firsthand the benefits of having women undergo regular screenings to check for breast cancer. Mammograms are the best tool we have to find breast cancer earlier, when it’s easier to treat, and tomosynthesis technologies have greatly improved our ability to identify potential cancers.
Despite these positive developments, comes a challenge: Women must sift through a lot of conflicting information about mammography:
- When should I start screening for breast cancer?
- What kind of mammogram technology should I opt for?
- How often should I be screened?
- When is it OK to stop having mammograms?
In this article, we’ll explore these important aspects of mammography:
- Screening mammograms vs. diagnostic mammograms
- Recommended ages for mammograms
- Digital and 3D-like mammography
- Dense breasts and mammograms
- Other imaging technologies
- Reducing anxiety during and after the imaging process
If you’re interested in undergoing breast imaging at CTCA®, or if you’ve been diagnosed with breast cancer and want a second opinion, call us or chat online with a member of our team.
The most important thing for women to know is there’s no reason to be scared of having a mammogram. While women should be familiar enough with their bodies to detect lumps or other concerning changes when performing manual self-examinations, that is no substitute for annual mammograms. Mammography is an important detection tool capable of spotting abnormalities that aren’t apparent by touch or sight.
Mammography basics
Performed by a specially trained technologist, mammography involves taking pictures of the breast using a special X-ray machine. A woman, or in certain instances a man, stands at the machine and places one of his or her breasts on a plastic plate. The breast is then compressed against the plate by another plate while the X-ray is taken. The more compression, the flatter the breast and the easier it is to spot abnormalities. The procedure is then repeated from a second view, and then the two views are repeated for the other breast.
Screening vs. diagnostic mammography
Women may have either a screening mammogram or a diagnostic mammogram, depending on the reason for the breast exam.
Most routine breast exams are performed for screening purposes, to check for signs of cancer in asymptomatic patients. The mammogram is designed to identify abnormal growths, but this may include benign growths, too. You may be called back for additional tests if the images detect unexplained abnormalities. In that case, you may undergo an ultrasound or biopsy, usually preceded by a second mammogram—this time a diagnostic mammogram.
A diagnostic mammogram is performed when suspicions have been raised about the potential for breast cancer—whether it’s discharge, a lump or other concerning sign you may have noticed during a self-exam, or abnormal results from a screening. While the process for undergoing a diagnostic mammogram is very similar to a screening mammogram, it’s performed, evaluated and read in very different ways. This exam may require taking additional images to determine the shape, density and borders of any mass, or zooming into specific areas for a closer look. That’s why diagnostic mammograms typically take a bit longer than the 10 to15 minutes a screening mammogram takes.
When to start annual screenings
Screening mammograms should be incorporated regularly into every woman’s annual checkup during a certain period of her life, even if she hasn’t been deemed a high risk for the disease. But many women find it difficult to determine when to start screening or how often they should have them, because major medical organizations differ, sometimes widely, on their recommendations.
Many studies have documented that if a woman is not considered at high risk for developing breast cancer, her chances of dying from breast cancer are greatly reduced if she starts having mammograms at age 40 and continues with yearly screenings. That’s the recommendation of the American College of Radiology and the Society of Breast Imaging, and I concur with them.
The U.S. Preventive Services Task Force says women who are not at high risk of breast cancer can wait to age 50 to begin mammography screenings, repeating them every two years after that. However, the science doesn’t back up those recommendations and may increase the time a cancer goes undetected—potentially leading to worse outcomes and fewer treatment options.
Age recommendations also differ for high-risk patients, who may have family histories of breast cancer or genetic mutations linked to breast cancer. These women would likely begin screenings earlier and may have them more often. In determining the timing and frequency of these exams, women in high-risk categories have other factors to consider, such as the age at which their mother or other close blood relative developed breast cancer. These decisions should be made in consultation with your doctor. If you don’t know whether you’re at high risk, the American Society of Breast Surgeons recommends undergoing a formal risk assessment for breast cancer starting at age 25.
While there’s no specific age to stop having screening mammograms, I tell my patients to continue screening for breast cancer as long as they don’t have life-limiting comorbidities (such as heart disease or another malignancy) or have a life expectancy of less than 10 years. As you get older, say about 70 or 75, the risk of breast cancer tends to decrease, so mammograms become less important at those ages.
The digital era of mammography
When mammography first debuted in the 1970s, small cassettes containing X-ray film were used to record the breast image. Since then, almost all mammography in the United States has moved from film screen to digital mammography.
Digital mammography emerged in the early 2000s, and by 2010, most hospital radiology departments had switched over to the newer technology. The image quality is much easier to control, providing better imaging of abnormalities, which reduces the likelihood of having to repeat the image-taking process. We can also upload the images onto a computer, which gives radiologists the ability to magnify and focus on areas of concern. Computers also make it easier for doctors to compare new mammograms to previous results. In some cases, computers with artificial intelligence are able to perform their own analysis of the images and identify areas of concern.
Why get tomosynthesis, and when?
Digital technology has also improved, especially with the development of digital breast tomosynthesis (DBT). You may hear tomosynthesis described as 3D mammography, but that’s not quite accurate. Tomosynthesis is 3D-like, but it’s not truly 3D.
During a traditional digital mammogram, doctors take one two-dimensional projection of the breast from above—we call it the CC, or craniocaudal, view—and another taken from the side, called the MLO or mediolateral oblique view.
Tomosynthesis uses an X-ray tube that moves in an arc around the breast to capture multiple images, then a computer stitches those images back together to give us a 3D representation of the breast. It’s not truly 3D because it’s still using slabs of information, or pieces of information that the computer pieces back together. This process can be performed using either the top view, the side view or both.
Digital tomosynthesis excels at what’s most important in mammography: It’s sensitive enough to find an abnormality and specific enough to separate the abnormality from the overlying tissues, allowing us to see subtle masses and architectural distortion often found with early cancer.
Most practices that perform extensive mammography have turned to tomosynthesis as their primary methodology for screening mammography. At CTCA, we typically combine a top view using a two-dimensional digital mammogram and the side view using tomosynthesis. Since tomosynthesis results in a slight increase in radiation exposure for the patient, this combination approach allows us to strike a compromise between concerns about exposure and the need to get the best images possible.
If red flags are identified during an initial screening exam, we ask the patient to return for additional images—including possibly a tomosynthesis involving the top view—to determine whether an ultrasound, magnetic resonance imaging (MRI) or biopsy may be needed.
The benefit of tomosynthesis is that it separates the overlapping tissues. In a traditional mammogram, an abnormality may be blocked from view by normal breast tissue, making it difficult to tell the difference between the two. With tomosynthesis, visualizing the different slices and slabs allows you to separate the normal from the abnormal, increasing our ability to detect abnormalities and decreasing call back rates. If doctors see something concerning on tomosynthesis, a follow-up ultrasound will likely be recommended.
From there, a biopsy, which involves the surgical removal of breast tissue, is the next step to confirm a cancer diagnosis.
Interpreting a mammogram
When radiologists examine mammograms, they look for certain characteristics that may indicate the presence of cancer.
The first are calcifications, which are little areas of calcium that show up as bright white specks in the breast’s soft tissue. The vast majority of these calcifications are benign, but some have a fairly characteristic pattern that’s associated with early cancers. These may indicate ductal carcinoma in situ (DCIS), which is the most common type of noninvasive breast cancer and starts in the milk duct. Other calcifications may also be associated with a more aggressive malignancy.
When we evaluate breast calcifications, we’re counting them and determining their pattern, examining each calcification to determine whether it’s benign.
We also look for any kind of mass or asymmetry. Tomosynthesis helps significantly with identifying a mass, because it separates the abnormality from the overlying breast tissue. You can see a mass on multiple views, while an asymmetry may just show up on one view. An asymmetry is a difference in the appearance of one part of the breast from other parts, or from the other breast, and may be an indication of cancer.
One of the most significant ways to detect breast cancer is to compare a new mammogram to those taken in the past. That’s another reason why annual screenings are so important. Something that might not stand out on a single mammogram may take on a whole new meaning when compared with past results.
The importance of breast density
When you undergo a mammogram, you’ll probably be told about the density of your breasts. Some states require mammogram results to include information about breast density, because the denser the breast, the higher the cancer risk. Cancer in a dense breast is also more difficult to spot on a mammogram.
Women’s breasts are divided into four categories for mammographic purposes, based on the amount of glandular tissue they contain. Your breasts typically become less glandular, or less dense, as you as you age, becoming fattier over time—although some women continue to have glandular breasts even as they get older.
The breast types are:
Type A: Breasts with extensive fatty tissue that are less than 10 percent glandular tissue
Type B: Mixed-density breasts that contain between 10 percent and 50 percent glandular tissue
Type C: Dense breasts that have between 50 percent and 75 percent glandular tissue
Type D: Extremely dense breasts that are more than 75 percent glandular tissue
We recommend that women with dense or extremely dense breasts, roughly 40 percent of all women, undergo either an ultrasound exam to complement mammography, or maybe an MRI. If you have dense breasts, discuss with your doctor which imaging procedure is best for you.
Other tests for breast cancer
Mammography isn’t the only tool used to detect breast cancer. In fact, researchers continue to explore other technologies, looking for a tool that may not require compression, to reduce the pain and discomfort some women experience during mammograms.
Options include:
MRI: An MRI is one test that works as well as or even better than mammography. The challenge with MRIs is they’re more expensive to perform, and they may cause discomfort in other ways—requiring, for example, patients to lie very still on their stomach for 15 minutes or longer.
Abbreviated breast MRI: In recent years, this new tool has allowed for a shorter sequence that usually takes less than five minutes. Some in the medical community are actively calling for abbreviated breast MRIs to be adopted as a screening tool, particularly for patients with denser breasts.
Molecular breast imaging (MBI) exams: These procedures include contrast enhanced spectral mammography (CESM), which injects an iodinated contrast material intravenously to assess for any kind of asymmetry that may be cancer. This is usually performed after a standard mammogram. Breast-specific gamma imaging (BSGI) is another molecular imaging procedure, this one uses an intravenous injected radionuclide and takes images that measure cellular activity in the breast. Activity that measures higher than background levels would raise the suspicion of cancer. Molecular imaging tests help doctors determine whether a breast biopsy is needed. Most times, a mammogram that detects asymmetry or a mass would be followed by a diagnostic ultrasound, which is very good at detecting cancerous lesions. Most practices only perform CESM or BSGI in cases where doctors aren’t sure of a diagnosis, even after an ultrasound.
Imaging technologies are critical to effective detection and treatment of breast cancer. The best chance to ensure a successful outcome is to take seriously the recommendation for annual mammograms beginning at age 40, or, for those at higher risk, the schedule set up in consultation with your doctor. It doesn’t make sense to put off having mammograms that could save your life.
The women’s imaging care teams at CTCA include technologists who handle the actual mammography, radiologists who interpret the images and direct any additional testing, and nurse navigators who help coordinate the communication between you and your care team. Our nurse navigators also provide counseling on scheduling and other educational information, and will answer the many questions you may have.
CTCA’s goals: Increasing comfort, reducing anxiety during and after the imaging process
At CTCA, we’re sensitive to making patients feel comfortable during their mammograms and reducing their anxiety levels afterwards—by moving quickly to determine whether any abnormality is cancer.
Our women’s care imaging teams focus on getting you in and out on schedule, while providing comfortable waiting rooms, dressing rooms and procedural areas. Because we have a smaller volume of screening patients, we don’t tend to get backed up, so we can spend more time ensuring each patient has that personal, one-on-one attention that’s a lot harder to offer in a bigger facility.
During screening mammography, we usually test from two views, from above using the traditional mammography and a side view using tomosynthesis. The tight compression, which may be uncomfortable, lasts for 10 to 15 seconds for each view of each breast, or typically less than a minute total.
You may be wondering: Why come to a cancer center such as CTCA for your screening when you could go to a local imaging center or hospital? It’s really about having peace of mind knowing that if something abnormal turns up, you’re in the hands of medical professionals who are experienced in identifying early cancers. Because we treat cancer every day, all day, our sensitivity for finding subtle abnormalities on a screening exam makes us well equipped to determine what additional tests should be ordered, or not.
If the mammography identifies a suspicious abnormality, we call our patients back within a matter of days, not weeks, for additional testing. All procedures—MRIs, ultrasounds, even biopsies—are typically performed on the same day, all under one roof, so you don’t have to worry about keeping track of multiple appointments. Should your mammography lead to a breast cancer diagnosis, our speed-to-care model allows us to be able to develop a personalized, comprehensive treatment plan with the urgency you deserve.
Each CTCA comprehensive care and research center has a dedicated Breast Cancer Center, staffed by multidisciplinary teams of breast cancer experts who have training and experience in the broad spectrum of diseases, from ductal carcinoma in situ to more complex diseases like triple negative and inflammatory breast cancer. Our breast surgeons also offer microsurgical approaches such as nipple-sparing mastectomy and reconstructive flap surgery, and our radiation oncologists employ technologies designed to reduce the risk of radiation exposure to the heart and other critical organs.
Wherever you decide to get your mammography screenings, the most important takeaway is to get them regularly, and to pay attention to abnormal changes in your breast. We’ve come a long way in the diagnosis and treatment of breast cancer, and early detection—thanks in large part to advances in mammography—has been key.
If you’re interested in undergoing breast imaging at CTCA, or if you’ve been diagnosed with breast cancer and want a second opinion, call us or chat online with a member of our team.
