By now, cancer patients should know what they need to do to protect themselves from COVID-19. New variants and subvariants continue to pose a threat to cancer patients and others with compromised immune systems. Those same rules will apply in the upcoming flu season, which usually peaks between December and February. Now cancer patients need to be vigilant about a new disease caused by a virus that has health care agencies raising red flags: monkeypox.
While the disease was once considered rare, the U.S. Centers for Disease Control and Prevention (CDC) now says it’s “tracking an outbreak of monkeypox that has spread across several countries that don’t normally report monkeypox, including the United States.” New cases of the virus have been reported in 87 nations, 80 of which have little or no history of previous cases. The World Health Organization has declared the monkeypox contagion a global health emergency.
Thousands of U.S. patients have been diagnosed, prompting the White House to declare a public health emergency. New York, California and Illinois have declared states of emergency because of the monkeypox outbreak, and the New York City Health Department has opened a vaccine clinic. Hundreds of monkeypox infections also have been reported in Florida and Georgia.
In this article, we’ll take a closer look at monkeypox and what cancer patients, their family members and caregivers can do to protect themselves. Topics include:
- What is monkeypox?
- How does it spread?
- What are the symptoms and treatment?
- What’s the threat to cancer patients?
- Is there a vaccine?
- How can cancer patients protect themselves?
- Patient safety at Cancer Treatment Centers of America® (CTCA)
If you’ve been diagnosed with cancer and are interested in a second opinion about your diagnosis or treatment options, call us or chat online with one of our team members.
What is monkeypox?
Monkeypox is an infection caused by a virus that’s in the same family as smallpox. The disease was first discovered in 1958 in Denmark in a colony of monkeys shipped from Singapore and used for research. But the true origins of the disease are unknown. The first case in humans was diagnosed in 1970 in the Democratic Republic of Congo. Most cases have been diagnosed in African countries.
In 2003, a case of monkey pox was reported in a 3-year-old Wisconsin girl who was bitten by a prairie dog. Within two months, 72 people were diagnosed in Wisconsin and Indiana. The cases were traced to a shipment of exotic animals imported from Ghana in west Africa. That outbreak was contained in a matter of months.
How does it spread?
Monkeypox is consider a zoonotic virus, meaning it can be spread from animals to humans and back again. During the recent outbreak, however, human-to-human contact has allowed the monkeypox virus to proliferate.
The virus is transmitted by:
- Intimate contact, such as hugging or kissing
- Oral, anal or vaginal sex or sexual contact, although it’s not considered a sexually transmitted disease
- Direct contact with skin rashes, scabs or secretions
- Direct contact with body fluids
- Close contact with respiratory droplets
- Direct contact with clothing or objects that had been touched by an infected person
What are the symptoms and treatment?
Symptoms of monkeypox may include:
- An itchy rash, lesions, pimples or blisters on the skin
- Fever and/or chills
- Headache
- Muscle aches and pains
- Swollen lymph nodes
- Fatigue
- Sore throat, cough or congestion
Symptoms may vary by patient. Some patients may get a rash before other symptoms, or vice versa. Symptoms may appear in as little as four days or as long as three weeks after exposure and may last up to four weeks.
Specific treatments are not available for monkeypox. Antiviral medications may be recommended for people with compromised immune systems, including cancer patients.
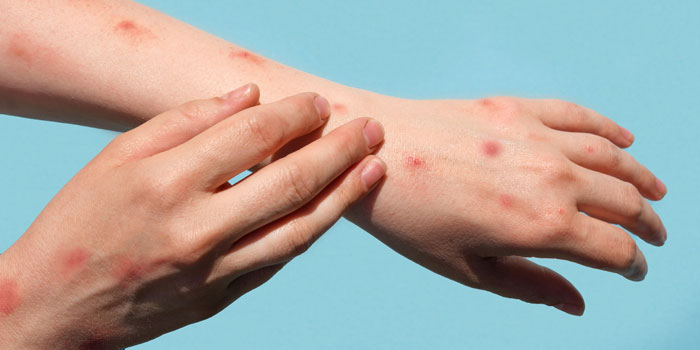
Why is monkeypox a threat to cancer patients?
Cancer and its treatments may attack, alter or weaken the immune system in a variety of ways, making patients more vulnerable to viruses and other diseases. For instance:
Blood cancers may damage or overpower immune cells or inhibit the body’s ability to produce new and healthy immune cells.
Chemotherapy drugs are designed to kill fast-growing cells like most cancer cells. But the treatment may also kill normal fast-growing cells in bone marrow, which produces immune cells.
Immunotherapy drugs boost the immune system to help it attack cancer cells. But overactive immune cells may also attack healthy cells. And a type of immunotherapy called CAR T-cell therapy may also damage or exhaust B-cells and affect the body’s ability to produce antibodies.
Stem cell transplants infuse the body with new healthy cells but require intense pre-treatment regimens that essentially strip the body of its immune cells.
Monkeypox may produce more severe symptoms in cancer patients and other immunodeficient people, though most cases do not require hospitalization. The disease is rarely fatal.
The CDC recommends that people infected with monkeypox isolate themselves for the duration of their illness. For cancer patients, that raises the potential of missing or delaying diagnostic or treatment appointments until they’ve recovered. Consultations and follow-up visits may be done remotely via telehealth.
“Any virus can be more of a threat to cancer patients,” says Suji Mathew, MD, Infectious Disease Physician and Chief of Medicine at CTCA® Atlanta. “If a cancer patient, caregiver or family member thinks they’ve been exposed, they should contact their care team member right away and consider going to the ER or hospital if they develop symptoms like fever, confusion, swollen glands and worsening rash or pain.”
Is there a vaccine?
There’s no specific vaccine for monkeypox, but the smallpox vaccine may help prevent infection.
The CDC recommends vaccinations for:
- Health care and medical laboratory professionals
- People who are sexually active with multiple partners
- Those who may have been in contact with someone with monkeypox
How can cancer patients protect themselves?
Aside from vaccination, experts advise taking steps to prevent monkeypox by avoiding exposure to the virus that causes it. Dr. Mathew recommends these steps:
- Avoid contact with infected animals, especially sick or dead animals.
- Avoid contact with bedding and other materials contaminated with the virus.
- Thoroughly cook all foods that contain animal meat or parts.
- Wash your hands frequently with soap and water.
- Avoid contact with people who may be infected with the virus.
- Practice safe sex, including the use of condoms and dental dams.
- Wear a mask that covers your mouth and nose when around others.
- Clean and disinfect frequently touched surfaces.
- Use gloves, face masks and other personal protective equipment when caring for people infected with the virus.
Patient safety at CTCA
Patient safety is a top priority at CTCA. While no cases of monkeypox have been reported among CTCA patients or staff, we take disease outbreaks of any kind very seriously and make sure our doctors, nurses and staff remain vigilant for symptoms, practice recognized safety protocols to prevent infection and know what to do in when a patient onsite is diagnosed with an infection.
CTCA took extraordinary measures during the COVID-19 pandemic to reduce the risk of patients and staff getting infected. Since COVID-19 remains a threat to cancer patients and others with compromised immune systems, CTCA consistently meets and exceeds necessary safety protocols. Precautions and protocols we've implemented include:
- Requiring masks for all visitors and staff
- Using enhanced cleaning and disinfecting measures
- Encouraging social distancing for staff and visitors
- Offering telehealth visits to qualifying patients through CTCA Anywhere®
- Offering home treatments with our Oncology Clinic at Home program
- Limiting visitors to adults over 18
If you’ve been diagnosed with cancer and want a second opinion about your diagnosis or treatment options, call us or chat online with one of our team members.