

This page was reviewed under our medical and editorial policy by
Maurie Markman, MD, President, Medicine & Science
This page was updated on June 21, 2022.
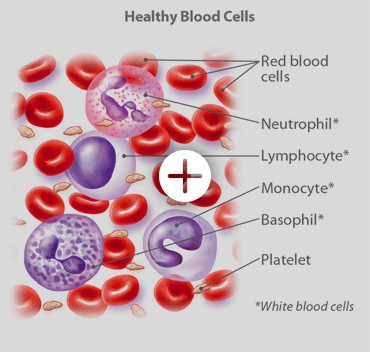
Most blood cancers, also called hematologic cancers, start in the bone marrow, where blood cells are produced. Blood cancers occur when abnormal blood cells grow out of control, interfering with the function of normal blood cells, which fight off infection and produce new blood cells.
This article will cover:
The three main types of blood and bone marrow cancer are leukemia, lymphoma and myeloma.
Leukemia is a blood cancer that originates in the blood and bone marrow. It occurs when the body creates too many abnormal white blood cells and interferes with the bone marrow’s ability to make red blood cells and platelets.
Non-Hodgkin lymphoma is a blood cancer that develops in the lymphatic system from cells called lymphocytes, a type of white blood cell that helps the body fight infections.
Hodgkin lymphoma is a blood cancer that develops in the lymphatic system from cells called lymphocytes. Hodgkin lymphoma is characterized by the presence of an abnormal lymphocyte called the Reed-Sternberg cell.
Multiple myeloma is a blood cancer that begins in the blood’s plasma cells, a type of white blood cell made in the bone marrow. Learn about the stages of multiple myeloma.
Less common forms of blood and bone marrow cancers, and associated disorders, include those listed below.
Myelodysplastic syndromes (MDS): These are rare conditions that may result from damage to blood-forming cells in the bone marrow.
Myeloproliferative neoplasms (MPNs): These rare blood cancers occur when the body overproduces white blood cells, red blood cells or platelets. The three main subcategories are essential thrombocythemia (ET), myelofibrosis (MF) and polycythemia vera (PV).
Amyloidosis: This rare disorder, characterized by the buildup of an abnormal protein called amyloid, is not a form of cancer. But it is closely associated with multiple myeloma.
Waldenstrom macroglobulinemia: This is a rare type of non-Hodgkin lymphoma that starts in B cells.
Aplastic anemia: This rare condition occurs when key stem cells are damaged and can only be treated with a bone marrow transplant.
Some common bone marrow and blood cancer symptoms include:
Blood cancers are caused by mutations in the genetic material—the DNA—of blood cells. Other risk factors vary based on the specific type of blood cancer.
Risk factors for developing acute myeloid leukemia (AML), the most common form of leukemia in adults, include:
Risk factors for developing Hodgkin lymphoma include:
Risk factors for developing non-Hodgkin lymphoma include:
Risk factors for developing multiple myeloma include:
A diagnosis often starts with a physical examination to check the patient's general health. The care team reviews the patient's health history, examines his or her body and lymph nodes, and looks for signs of infection or bruising.
Different types of tests and procedures may be used to diagnose blood cancer. What each patient needs depends on the type of blood cancer suspected. The care team may recommend testing and evaluate all the results along with the patient to make a diagnosis.
A biopsy is a test that collects samples of cells for examination by a pathologist in a laboratory. For some types of blood cancer, like lymphoma, the patient may need a lymph node biopsy that obtains a sample of lymph tissue or an entire lymph node.
Testing the bone marrow, where blood cells are formed, can help diagnose certain types of blood cancer. Doctors use a procedure called a bone marrow aspiration to remove a small sample of bone marrow, blood and bone from either a hip bone or breastbone. The sample is sent to a lab and checked for abnormal cells or changes in genetic material.
Imaging scans are more helpful for some types of blood cancer than others. A scan may spot an enlarged lymph node, which is a common symptom of lymphoma, but it’s not usually used to diagnose leukemia, a blood cancer that doesn’t cause visible tumors. Still, scans may help whether cancer has affected other parts of the body.
Scans include:
Certain types of scans are used during biopsies to help pinpoint the area to be sampled.
A complete blood count (CBC) shows the cell count of different components of blood, such as white blood cells, red blood cells and platelets.
Blood chemistry tests measure levels of key substances in the blood. Abnormal levels of certain proteins, for example, may offer information about the patient's condition. If multiple myeloma is suspected, doctors may want to check the patient's blood calcium level. For possible lymphoma, an enzyme called lactate dehydrogenase (LDH) may be measured.
Treatment for blood and bone marrow cancers depends on the type of cancer, the patient's age, how fast the cancer is progressing, where the cancer has spread and other factors. Some common blood cancer treatments for leukemia, lymphoma, and multiple myeloma include those listed below.
Stem cell transplantation: A stem cell transplant infuses healthy blood-forming stem cells into the body. Stem cells may be collected from the bone marrow, circulating blood and umbilical cord blood.
Chemotherapy: Chemotherapy uses anticancer drugs to block the growth of cancer cells in the body. Chemotherapy for blood cancer sometimes involves giving several drugs together in a set regimen. This treatment may also be given before a stem cell transplant.
Radiation therapy: Radiation therapy may be used to destroy cancer cells or to relieve pain or discomfort. It may also be given before a stem cell transplant.
Learn more about leukemia treatments, Hodgkin lymphoma treatments, non-Hodgkin lymphoma treatments and multiple myeloma treatments
A blood cancer prognosis varies based on the type and other factors, including the patient's overall health, age and response to treatment.
According to the National Cancer Institute’s Surveillance, Epidemiology, and End Results (SEER) Program, the five-year relative survival rate (the percentage of people who were still alive five years after diagnosis) is 66.7 percent for leukemia—a number that has improved dramatically in the past 50 years. Other rates include:
Keep in mind that these survival rates are estimates, based on historical data and past treatments. Advances in medicine may make the patient's experience even more hopeful.