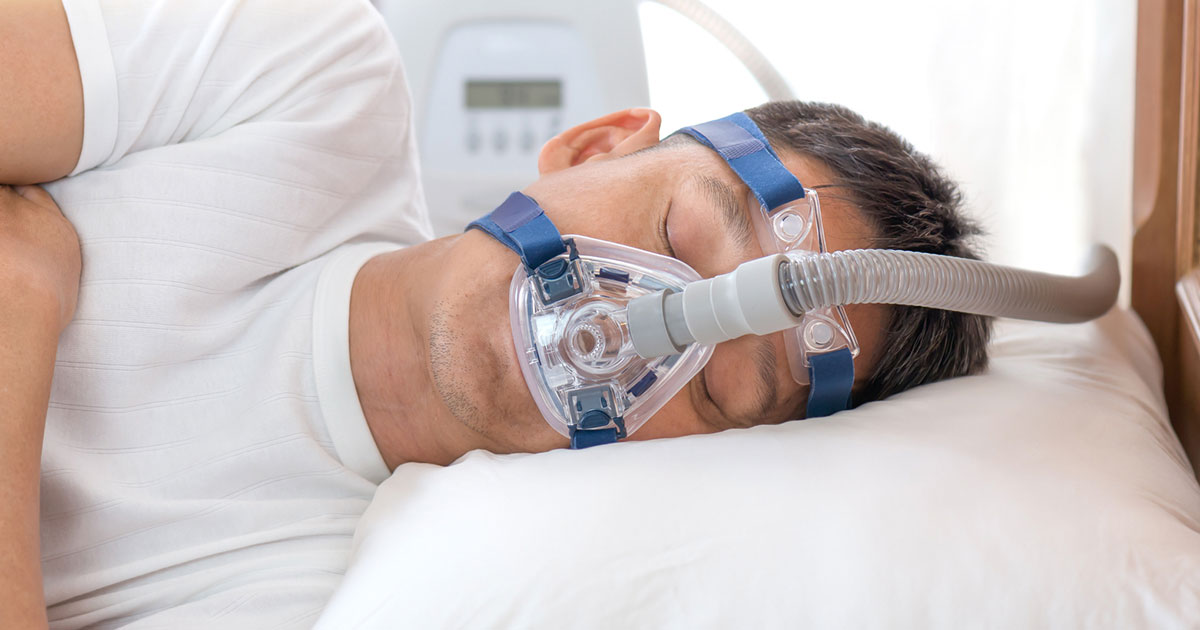
If you snore or find yourself gasping for air during sleep, you may have obstructive sleep apnea (OSA). It’s a common disorder, affecting up to 13 percent of the global population, that causes people to stop breathing several times a night as a result of partial or complete obstruction of the airways.
But OSA is more than simply a bedtime nuisance that interrupts a good night’s sleep and leaves you feeling sleepy during the day. OSA has also been linked to an increased risk for certain cancers, as well as stroke, diabetes, cardiovascular conditions (such as blood clots and congestive heart failure) and cognitive decline, studies show.
Risk factors for OSA include:
- Being overweight or obese
- Having diabetes
- Smoking
- Drinking a lot of alcohol
Treatment typically includes the use of CPAP machines. Short for continuous positive airway pressure, CPAP devices are designed to keep the airways open during sleep.
Some studies have found that CPAP therapy may reduce the risk for cardiovascular conditions, but the research is mixed on whether it reduces cancer risk. In fact, some research has found certain CPAP machines may actually increase cancer risk, according to the U.S. Food and Drug Administration (FDA). But scientists say more research is needed to confirm the risks and benefits of treating OSA.
To help you understand the cancer risks associated with OSA, and what you can do to reduce them, this article answers several common questions about the condition:
- What is sleep apnea?
- What’s the link between sleep apnea and cancer?
- Does treating sleep apnea reduce cancer risk?
- Do CPAP machines cause cancer?
- What can OSA patients do to lower their cancer risk?
- Cancer, its treatments and sleep issues
If you’ve been diagnosed with cancer and are interested in a second opinion on your diagnosis and treatment plan, call us or chat online with a member of our team.
What is sleep apnea?
Sleep apnea is a potentially serious sleep disorder in which breathing repeatedly stops and starts overnight. Unlike occasional insomnia or sleeplessness, apnea is a chronic condition that may result in oxygen deprivation to the body, organs and brain—raising the risk for cancer, dementia and cardiovascular problems. The main types and causes of sleep apnea are:
- Obstructive sleep apnea (OSA), the more common form that occurs when throat muscles relax
- Central sleep apnea, which occurs when the brain doesn't send proper signals to the muscles that control breathing
- Complex sleep apnea syndrome, also known as treatment-emergent central sleep apnea, which occurs when someone has both OSA and central sleep apnea
The most common sleep apnea symptoms include loud snoring, gasping for air during sleep and feeling tired even after a full night’s rest. Other symptoms include:
- Episodes in which you stop breathing during sleep (reported by someone who witnesses it)
- Dry mouth upon awakening
- Morning headache
- Difficulty staying asleep
- Excessive daytime sleepiness
- Difficulty paying attention while awake
- Irritability
If you have these symptoms, talk to your doctor about undergoing a sleep apnea test at a specialized center or clinic. Such evaluations typically involve spending a night in a clinic while technicians monitor your sleeping patterns, arm and leg movements, blood-oxygen levels and heart, lung and brain activity. Some people may undergo a simplified home test. You may also choose to participate in a sleep study, where your condition and symptoms are evaluated and treated with new therapies undergoing testing.
Sleep studies have found some obstructive sleep apnea treatment options may help ease symptoms and may even prevent heart problems and other complications.
What’s the link between sleep apnea and cancer?
Numerous studies have tied sleep apnea to an increased risk for cancer, as well as other health conditions. But until recently, it wasn’t clear whether those risks were due to sleep apnea itself or other risk factors associated with the condition—such as obesity, cardiovascular conditions or unhealthy lifestyles.
But a series of recent landmark studies reported by the European Respiratory Society found people with OSA are at an increased risk of cancer—as a result of oxygen deprivation caused by the disorder—as well as a decline in mental processing (particularly in older people) and the development of potentially serious blood clots in the veins.
The researchers took into account factors that may affect the results of the study, such as body size, other health problems and socio-economic status. They also measured the severity of OSA in study participants, based on the number of breathing disturbances during sleep and how many times an hour they experienced oxygen deprivation—where oxygen in the blood falls by at least 3 percent for 10 seconds or longer.
Participants who had been diagnosed with cancer had a higher prevalence of OSA. The study also determined those with lung cancer, prostate cancer and melanoma— had higher levels of oxygen deprivation during sleep.
The researchers said the findings highlight the need to consider “untreated sleep apnea as a risk factor for cancer and for doctors to be aware of the possibility of cancer when treating patients with OSA,” but stopped short of recommending cancer screening for all people with OSA.
Does treating sleep apnea reduce cancer risk?
Although research has linked untreated sleep apnea to cancer, common sense suggests treating the sleep disorder would reduce cancer risk. But study findings have been inconclusive at best on whether the use of CPAP sleep apnea machines—the most common therapy approach—reduces cancer risk. Such devices deliver enough air pressure to keep users’ upper airway passages open, through a mask or mouthpiece, to prevent nighttime snoring and apnea.
Studies have found CPAP users lower their risks for heart disease, diabetes and cognitive disorders. But a landmark sleep study published recently in the European Respiratory Journal found, for instance, that people who used CPAP machines were not less likely to develop cancer. For the study, researchers tracked patients who were prescribed CPAP for OSA and had no history of cancer before the study or during the first year of CPAP use. After five years, roughly the same percentage of study participants developed cancer.
“CPAP therapy in OSA patients was not associated with a reduction in all-cancer incidence,” the researchers concluded. But they added that more research is needed to determine whether CPAP machines may reduce the risk of specific cancers.
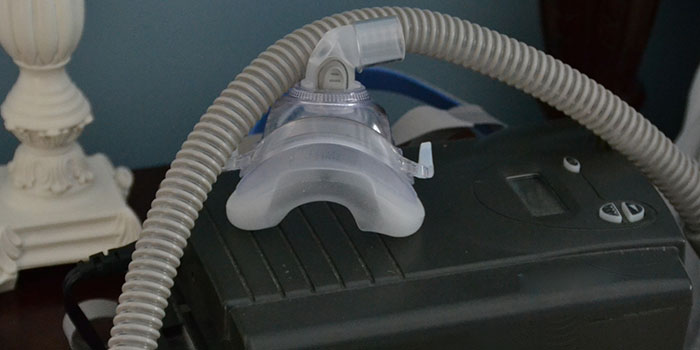
Do CPAP machines cause cancer?
The FDA has warned that certain CPAP machines may be linked to cancer.
In 2021, an FDA warning noted certain CPAP devices were recalled after being linked to an increased cancer risk. The risk was associated with the suspected breakdown of the foam used in certain ventilators and CPAP or similar machines, potentially causing the devices to malfunction or lead to the release of trace amounts of toxic particulate matter that may be inhaled or swallowed.
The FDA has requested additional information from the manufacturer about the cause of the issues and asked them to provide informed recommendations to patients, caregivers and health care professionals.
What can OSA patients do to lower their cancer risk?
Treatments for sleep apnea vary, depending on the severity of the case. For instance, several forms of positive airway pressure (PAP) therapy, other than CPAP, may be used to treat apnea, keeping the airways open as the patient sleeps by delivering a stream of air through a facemask.
- APAP: Auto titrating positive airway pressure therapy automatically raises or lowers the air pressure as needed during sleep.
- BiPAP: Bilevel positive airway pressure (BiPAP) devices have two alternating levels of pressure and may work better for people who have difficulty using CPAP or APAP.
Using supplemental oxygen or oral appliances designed to keep the throat open may sometimes work for people with mild apnea. Treating other conditions—such as neuromuscular disorders—may also help ease apnea symptoms.
Other bedtime strategies that may help improve night sleep include those below.
Develop a routine. Get up and go to bed the same time every day. Develop bedtime rituals, such as listening to relaxing music, reading and doing relaxation exercises.
Reduce distractions. Use earplugs, a mask or bedroom-darkening curtains.
Don't take naps. Save the sleep for bedtime.
Use your bed for sleep and intimacy. Perform all other activities elsewhere.
Put down the phone. So-called blue light emitted by phones and tablets may delay melatonin production and disrupt sleep patterns.
Cut down on caffeine. Don’t drink coffee or caffeinated beverages after noon.
Quit smoking. Nicotine is a stimulant. Smoking may also increase snoring and sleep apnea.
Watch the alcohol consumption. A couple drinks may help you fall asleep. But when the alcohol wears off, you may waken and have difficulty going back to sleep.
Get moving. A run, brisk walk or vigorous workout early in the day may help you sleep better. But don’t exercise within four hours of bedtime.
Watch what you eat. A light, high-protein snack before bed is fine. But avoid going to bed too soon after a big meal.
Get out of bed. If you can't fall asleep within 20 minutes, get up and do something until you feel sleepy.
If you suffer from apnea and can’t find a workable treatment, speak with your doctor during your annual physical—particularly if you have new symptoms. Your doctor may recommend bloodwork and/or cancer screening.

Cancer, its treatments and sleep issues
A good night sleep has significant health benefits. It not only reduces your cancer risk but is especially beneficial for those diagnosed with cancer or other diseases.
For cancer patients, anxiety caused by uncertainty and fear about the future and decisions about treatment may cause stress that hampers sleep. The symptoms of cancer or the side effects of treatment, including certain medications, also may contribute to sleep problems.
Cancer patients are twice as likely to experience insomnia. Up to 80 percent of cancer patients have difficulty falling and/or staying asleep. Sleep apnea is more common among cancer patients, with almost 30 percent reporting fatigue.
Studies show a lack of sleep may contribute to poor outcomes for patients undergoing treatment. Sleep allows the body to relax and recover from daytime activities. Lack of sleep may depress the immune system and hamper recovery from illness.
Chronic sleeplessness may also alter the balance of cortisol and melatonin, two hormones that influence the behavior of cells. Cortisol regulates immune function, including the release of killer cells that help the body battle cancer. Melatonin, produced by the brain during sleep, may have antioxidant properties thought to help prevent damage to cells.
If you’ve been diagnosed with cancer and are interested in a second opinion on your diagnosis and treatment plan, call us or chat online with a member of our team.



