
Rising or elevated prostate-specific antigen (PSA) levels, an abnormal digital rectal exam (DRE), or both, may indicate the presence of prostate cancer, and having those conditions may lead your doctor to recommend a prostate biopsy. But controversy surrounding the PSA blood test and concerns about prostate biopsies cause many patients to ask:
- Should I get a prostate biopsy?
- Are the risks of a prostate biopsy worth it?
- Are there alternatives to a prostate biopsy?
- If I have prostate cancer, is treatment necessary if I’m not experiencing symptoms?
If you’re looking for answers to these questions, you may find conflicting and confusing information across the medical field, in the news and on prostate cancer websites. Some dispute the necessity of prostate cancer screening and discourage men from getting a PSA test to begin with. Others suggest that prostate cancer is overtreated and that the risks associated with biopsies and treatment aren’t worth the potential benefit.
While the 10-year survival rate of men with a diagnosis of prostate cancer is approximately 98 percent, prostate cancer remains the second leading cause of cancer deaths in American men. The American Cancer Society (ACS) estimates that 248,530 new cases of prostate cancer will be diagnosed in the United States in 2021 and that one in every 41 men diagnosed will die from the disease.
Not everyone should have a prostate biopsy, but prostate cancer remains a serious threat to men. Without undergoing a biopsy, a physician can’t determine whether you have prostate cancer. And if you do have prostate cancer, biopsy results may help determine how aggressive it is and the chance that it has or will spread outside your prostate—all of which in turn determines which treatment options may be appropriate for you.
A prostate biopsy is not risk-free, but we have methods, in addition to the PSA and DRE, that may help determine whether you need one. We also have tools that help reduce the risks of a biopsy and increase the chances of its accuracy.
To help you better understand this topic and whether you should get a prostate biopsy, this article will cover:
- Controversies and misconceptions surrounding prostate biopsies
- Benefits of getting a prostate biopsy
- Prostate biopsy risks
- How doctors determine whether a patient needs a prostate biopsy
- How we approach prostate biopsies and prostate cancer diagnosis at City of Hope
If you're interested in learning more about the diagnosis and treatment of prostate cancer, or if you'd just like to talk to someone at City of Hope about your cancer care, call us or chat online with a member of our team.
Controversies and misconceptions surrounding prostate biopsies
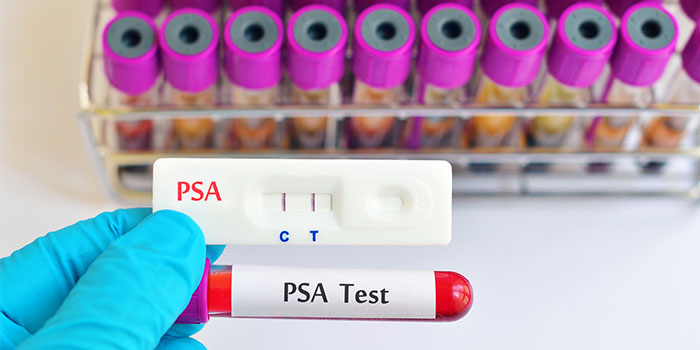
The PSA test measures the levels of PSA proteins in the body, and when it was first developed, it was quickly implemented by many physicians as a screening test for prostate cancer. The thought was that since PSA proteins are only produced by the prostate, elevated levels could be an indication of prostate cancer. As a result, most men with an abnormal PSA test underwent a prostate biopsy.
The increase in biopsies resulted in the number of advanced, untreatable prostate cancers decreasing significantly because more prostate cancers were caught earlier, when the disease is easier to treat. But the problem with many patients being diagnosed sooner was that some patients were being aggressively treated when they should have been monitored instead.
Though many in the field of urology believe it was flawed, a controversial study attempted to assess the benefits of the PSA test as a screening tool for prostate cancer, and its results led to the recommendation that most men shouldn't get the test because it didn’t appear to improve mortality rates from prostate cancer. This, combined with growing awareness that many cases of prostate cancer were being treated unnecessarily or prematurely, led to a reduction in prostate biopsies. This controversy led to a reduction in prostate cancer screening and an increase in the number of diagnoses of advanced prostate cancer.
Not all patients who have high PSA levels have cancer, but the PSA test, combined with a number of risk factors, remains one of the most reliable indicators we have to alert us to the possibility of prostate cancer.
Common objections from patients regarding prostate biopsies
Urologists often hear some common objections from patients after a prostate biopsy is recommended, and most of them stem from misconceptions about prostate cancer.
Many patients ask why they should get a prostate biopsy if they're not experiencing urinary symptoms. The reality is that the majority of patients with prostate cancers have no urinary symptoms. These symptoms are most commonly associated with an enlarged prostate, which is usually a benign condition not related to prostate cancer. If prostate cancer patients wait long enough to experience urinary symptoms, they tend to have advanced, difficult-to-treat cancer. The majority of prostate cancer patients show no symptoms of any kind when first diagnosed.
Another common objection from patients is that there‘s no history of prostate cancer in their family. While it's true the risk of prostate cancer increases if you have a family history of the disease, the majority of patients have no first-degree relatives with prostate cancer. Only about 20 percent of prostate cancers are familial.
Finally, many patients object to undergoing a prostate biopsy because they've heard about the procedure's risk of infection. While this risk is real, there are steps that can be taken to reduce the risk of infection. If your physician’s medical advice is that you should undergo a prostate biopsy, he or she feels the risk of living with undiagnosed prostate cancer is higher for you than the relatively small risk of infection from a biopsy.
Benefits of getting a prostate biopsy
A prostate biopsy is the only way to definitively determine whether you have prostate cancer and, if you do, how aggressive it is.
While prostate biopsies aren’t always conclusive, in general, a biopsy gives men the reassurance of knowing whether they have cancer or not. If you know you have prostate cancer, you’re more likely to be appropriately treated.
Appropriate prostate cancer treatment options depend on several factors, including the stage of the cancer, your age, your general health and which risk category your cancer falls into.
Localized prostate cancer (cancer that’s confined to the prostate) is categorized into six risk categories, which range from very low-risk to very high-risk. The risk group is determined by the stage of your cancer, your PSA levels and the Gleason score obtained from the biopsy pathology report. (Cancer that’s metastasized, meaning it’s spread outside the prostate, isn’t assigned to a risk category, because it’s already progressed to stage 4 disease.)
The National Comprehensive Cancer Network (NCCN) guidelines outline appropriate treatment options based on risk categories and whether the cancer has already metastasized.
Patients whose cancer is confined to the prostate and falls into the very low-risk and low-risk categories tend to have slow-growing cancers. Treatment options for these patients often include active surveillance, radiation therapy or surgery. Similar treatment options may be recommended to patients in the low-risk and favorable intermediate prostate cancer risk categories.
If you and your doctor have chosen active surveillance, you'll need to follow your doctor’s medical advice to monitor your cancer. Follow-up monitoring may include periodic PSA tests and DREs, imaging tests and a biopsy every one to two years.
The NCCN guidelines recommend immediate treatment for patients with high-risk disease or those patients whose cancer has metastasized.
We try to find the right balance in prostate cancer treatment. We don't want to overtreat a slow-growing cancer, but we also don't want to miss the window of opportunity to treat an aggressive cancer.
Prostate biopsy risks
There are risks associated with prostate biopsies, but physicians can take steps to reduce those risks. Risks and ways to manage them include:
Infection: The most serious risk of a prostate biopsy is the risk of infection, including urinary tract infections and, less commonly, sepsis. However, recent studies found that with appropriate interventions, such as administering a double course of antibiotics and taking other precautions, infection-related hospitalizations after prostate biopsy fell from 1.19 percent to 0.56 percent. It’s also possible to perform a test using a stool sample to determine which antibiotics may be suitable for you.
Bleeding: This risk is very low, and physicians reduce it further by making sure patients scheduled to undergo a prostate biopsy aren’t taking blood thinners.
Discomfort: Patients may also fear the procedure will cause discomfort. Your urologist will most likely use a local anesthetic to alleviate pain. If you don’t tolerate pain well and the fear of it causes you great anxiety, ask whether a short course of anesthesia during the procedure is possible. Because we’re a cancer hospital and we have the means to do so, I try to accommodate patients at CTCA® who have an extreme fear of the procedure when they request it.
Patients may experience some soreness in the rectum or scrotum afterwards.
Given these risks, physicians carefully assess each patient’s specific situation before recommending a biopsy.
How doctors determine whether to recommend a prostate biopsy

No two patients are alike, and a urologist needs to take many variables into account before recommending a prostate biopsy, including a patient’s:
- Age and life expectancy
- Urologic history
- Personal risk of infection
- Comorbidities (pre-existing health conditions)
- Change in PSA values across time.
The decision of whether to undergo a prostate biopsy should be determined after an individual conversation with your doctor during which he or she presents you with the big picture of your situation.
Compare, for example, the case of two 50-year-old men: One of them has been diagnosed with heart failure and is in poor overall health. The other has no pre-existing health conditions. I probably wouldn’t advise a prostate biopsy for the 50-year-old with heart failure because prostate cancer is unlikely to cause his death within the next five years.
But I would recommend that the healthy 50-year-old get a prostate biopsy, because even if his cancer isn’t aggressive right now, missing a prostate cancer diagnosis may result in his death from the disease in 15 years. In his case, it would be better to risk the prostate biopsy to catch the cancer early and improve his chances of long-term survival.
Additional tests that may aid prostate cancer diagnosis
There are few other diagnostic tools or tests, which can be performed before you have a prostate biopsy, that may help your physician gather more information about your specific case. These procedures may help determine the likelihood of the presence of cancer and its aggressiveness and increase the accuracy of a biopsy when performed. Those tests include:
4Kscore blood test is a molecular test that helps predict the likelihood and risk of a patient having aggressive prostate cancer. If you're a patient whose PSA values are borderline for a prostate biopsy or you have a condition that could be aggravated by a biopsy, your physician may use this test before to help determine whether you should get a biopsy or a repeat biopsy.
Urine sample test looks for biomarkers that may indicate the presence of prostate cancer cells in a patient's body. This test may also be helpful when trying to determine whether a patient should be rebiopsied or not.
Multiparametric MRI
The use of multiparametric MRI (mpMRI) imaging of the prostate gland before a biopsy has been a game changer in prostate cancer diagnosis, increasing the accuracy of biopsies over standard biopsies. The mpMRI doesn't replace the standard biopsy, but by improving its accuracy, it may help decrease the number of biopsies needed.
The mpMRI has a higher resolution than a standard prostate ultrasound. This increases the ability to see suspicious lesions in the prostate, providing additional targets for the biopsy to sample.
The mpMRI isn’t perfect, though. It has a false negative rate of about 40 percent because some cancer cells are too small to be detectable. So, even if your MRI is negative (meaning no lesions were found), we still recommend you undergo a prostate biopsy when your urologist recommends it. (Also note that while finding lesions on the prostate may indicate the presence of prostate cancer, an image can’t tell us whether the cancer is aggressive. Biopsy samples of the tissue are necessary for that determination.)
If the mpMRI shows an abnormality in your prostate, we can then sync the images obtained during the MRI with the images from the transrectal ultrasound (TRUS) of your prostate during the biopsy. This is called an MRI-fusion biopsy, and it provides us with a visual target of the sampling area in real time. We’re then able to take the standard, 12 random prostate tissue samples plus biopsy samples from areas that showed lesions (if any), guided by the MRI-fusion.
I've been recommending and performing MRI-fusion biopsies for the past seven years. Two years ago, the NCCN added it to its standard-of-care guidelines for initial prostate biopsy.
How we approach prostate biopsies and prostate cancer diagnosis at City of Hope
When you come to City of Hope for a prostate biopsy or a second opinion, you’ll have access to tests that may help increase the accuracy of each biopsy. Our team has expertise with these tests and procedures, allowing us to work quickly and efficiently.
If you’re diagnosed with prostate cancer, a multidisciplinary team of genitourinary experts, which may include a urologist, a urologic oncologist, a radiation oncologist and a medical oncologist, will review your case and develop a personalized plan based on your specific circumstances and needs.
Our cancer experts are skilled at assessing risk associated with each person’s circumstances. We give you the pros and cons of the treatment options available to you, allowing you time to talk with your team of doctors and other experts about those options.
Our cancer experts are also vigilant about what patients need and when they need it. We know that when men are told they have slow-growing prostate cancer, some of them won’t keep up with the necessary follow-ups, so we help keep them on track.
If you choose to receive treatment with us, you may benefit from our integrative approach to cancer treatment. Our multidisciplinary team works together to help prevent and manage the side effects of cancer and its treatment, providing supportive care services, such as:
Making your decision
Before you make a decision about whether to have a prostate biopsy, we recommend you have a conversation with your physician and ask:
- What’s my risk of undiagnosed prostate cancer?
- Are we doing all the necessary testing to appropriately perform a risk-benefit analysis of getting a prostate biopsy?
You may also want to consider getting a second opinion and, if possible, consult with a urologic oncologist.
It's important to remember that the statistics surrounding prostate cancer, its diagnosis and treatment are gathered at the population level. They are, in other words, generalizations. Individual patients, on the other hand, are more than just numbers.
When deciding whether to get a prostate biopsy, don't let generalizations about the procedure and the disease determine what's right for you. Make sure you’re getting the information you need about your individual circumstances to make an informed decision.
If you’d like to schedule a consultation with the multidisciplinary team of prostate cancer experts at City of Hope, call us or chat online with a member of our team.
