
If you’re like most men who’ve been diagnosed with prostate cancer, you’ve been told you have early-stage, localized prostate cancer, meaning the disease hasn’t spread beyond the prostate. You may have also been told that you have choices about what you want to do next.
Unless your cancer is aggressive, you’ve probably been presented with three treatment options:
- Active surveillance: Oncologists use this method for less aggressive prostate cancer. Your care team will runs test periodically to evaluate whether the cancer has progressed. If so, they may recommend additional treatment.
- Radiation therapy: This treatment uses targeted radioactive energy to reduce tumor size, destroy cancer cells and alleviate some cancer-related symptoms.
- Surgery: Typically, this involves a procedure called a prostatectomy, which removes the prostate and surrounding cancer cells.
If you aren’t comfortable with active surveillance (also called watchful waiting), or if your oncologist says it isn’t the right option for you, you may have to decide between radiation therapy and surgery to treat your cancer.
Many men want to know what’s the “best treatment” for their localized prostate cancer. But it’s a misconception that you have only one “better” or “safer” choice. In most cases, either radiation therapy or surgery is an equally good choice when we look at long-term survival.
We’ve heard of some physicians telling men of their prostate cancer diagnosis and asking them to make a treatment decision at the same appointment. But prostate cancer progresses slowly, so most men have time to think about their options and shouldn’t feel pressured into making an immediate decision.
How you feel about the “big three” possible side effects of treatment—urinary incontinence, sexual dysfunction and bowel health—may be the deciding factor for you.
It’s okay to say you’d like some time to think about your options and seek a second opinion. With a clear understanding of your options, you’re more likely to make a decision you’ll be comfortable with in the long run.
To help you through the process of making this decision, this article covers:
- Radiation therapy for localized prostate cancer
- Surgery for localized prostate cancer
- How to compare radiation vs. surgery for prostate cancer
- How prostate cancer staging and risk group affect treatment options
- What the research shows about radiation vs. surgery
- Get a second (or even a third) opinion
- Are surgery and radiation therapy ever used together?
- How we approach prostate cancer treatment at City of Hope®
If you’re interested in learning about treatment options for your prostate cancer, or if you’d just like to talk with someone about your cancer care, call us or chat online with a member of our team to schedule an appointment.
Radiation therapy for prostate cancer

If your care team is considering radiation therapy as part of your treatment regimen, you’ll work directly with a radiation oncologist. He or she will explain the specific type of radiation therapy recommended for your cancer and answer any questions you have.
Some prostate cancer patients wonder about the safety of this treatment. Thanks to scientific advances, radiation therapy techniques have improved over the years. More precise radiation delivery techniques are designed to help spare normal tissue from exposure and reduce the severity of side effects. In addition to the external delivery of radiation, we now also have internal delivery options. In some cases, courses of radiation treatment may be more intense and shorter in duration.
The development and use of hydrogel spacers—gel that’s inserted between the prostate and the rectum—may also reduce damage to tissue surrounding the prostate during radiation, which in turn helps to reduce treatment-associated side effects.
External beam radiation for prostate cancer
When most patients think of radiation therapy, they think of external beam radiation therapy (EBRT), in which a beam of radiation is directed at cancerous tissue from outside the body. Technological advances, such as intensity-modulated radiation therapy (IMRT) and image-guided radiation therapy (IGRT), allow radiation oncologists to use computer-controlled devices and image-guidance technology to see and target a three-dimensional image of the tumor, making the treatment more precise than ever before.
In the past, EBRT required 40-45 daily treatments. Now, 25-28 treatments are the norm. This type of protracted, fractionated (many sessions over a longer period of time) radiation therapy, however, is now generally considered to be less appropriate for low-risk and favorable intermediate-risk patients. Instead, hypofractionated techniques (brief, short-courses of radiation therapy) and brachytherapy techniques are generally more advisable for many patients.
Brachytherapy for prostate cancer
Brachytherapy is a form of internal radiation therapy. With this type of therapy, radiation is delivered to the prostate tumor inside the body via a catheter or another implantable device.
High-dose rate (HDR) brachytherapy uses radioactive Iridium-192 to deliver high doses of radiation to the prostate tumor. Treatments are short, sometimes requiring as few as five sessions. Brachytherapy radiation more tightly surrounds the tissues we’re targeting, which may help spare normal tissues.
Side effects of radiation for prostate cancer
The primary potential side effects of radiation treatment for prostate cancer include bowel problems, urinary problems and sexual function issues.
According to patient-reported outcomes measuring quality of life from men who participated in the 10-year, randomized Prostate Testing for Cancer and Treatment (ProtecT) trial, men who were treated with radiation reported little increase in urinary leakage after radiation therapy. They also reported less sexual dysfunction when compared to men who were treated with surgery. However, men treated with radiation reported a higher incidence of bowel problems, such as loose and bloody stools. These side effects are often short-term for most patients, but some experience long-term side effects.
Surgery for prostate cancer
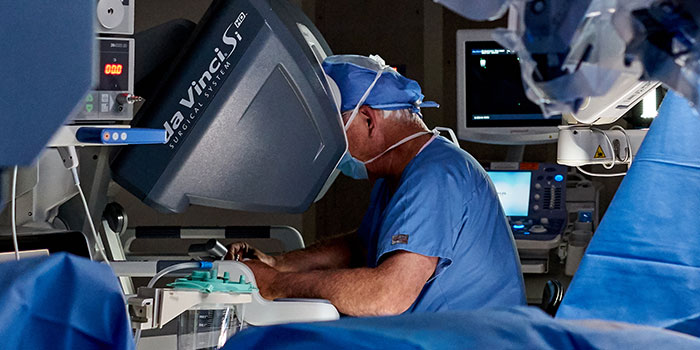
A radical prostatectomy is the surgical removal of the prostate. This procedure may be performed through traditional open surgery, which involves one large incision in the abdomen. Laparoscopic surgery using the robotic daVinci® Surgical System is a minimally invasive alternative. Robotic surgery only requires a few small incisions in the abdomen, which may result in reduced pain, lower risk of infection and a shorter hospital stay after surgery.
The technology associated with the robotic surgical system is designed to give the surgeon greater precision and control, which may help spare healthy tissue and one or two of the nerve bundles on the sides of the prostate. This often allows the patient to have better erectile function—in both the short term and long term.
Side effects of surgery for prostate cancer
The most commonly experienced side effects of surgery for prostate cancer are urinary incontinence and erectile dysfunction.
According to the patient-reported outcomes from men who participated in the ProtecT trial, men who underwent a radical prostatectomy experienced more sexual dysfunction and urinary problems than those treated with radiation therapy.
While many reported an improvement in the severity of their symptoms six months after surgery, these men continued to report poorer sexual quality of life six years after surgery compared to those who had radiation therapy.
Although men treated with radiation reported experiencing bowel function problems after treatment, the study participants who had a prostatectomy were generally able to undergo the procedure without experiencing any changes in bowel function after surgery.
How to compare radiation vs. surgery for prostate cancer
When trying to decide between radiation and surgery for localized prostate cancer, many men still ask whether one approach is “better” or “safer” than the other.
Research from the ProtecT trial shows us that radiation and surgery are good options, with the caveat that the specifics of your personal health condition could make one more advisable than the other. If that’s not the case, rest assured that you’re not at risk of making a terrible decision: Radiation and surgery are both solid options.
How to evaluate radiation vs. surgery comes down to understanding the disease and the research on treatment outcomes, getting a thorough understanding of your specific situation and then deciding which pathway you feel is right for you.
How prostate cancer staging and risk group affect treatment options
Your treatment choices are determined by several factors, including your cancer’s stage, aggressiveness and assigned risk stratification (commonly known as a risk group). Your age and current general health condition may also affect your choices.
Prostate cancer staging
Prostate cancer staging determines whether the cancer is confined to the prostate gland or whether there’s evidence of metastasis, meaning it’s spread to other areas of the body.
Tools and methods to determine staging may include the prostate-specific antigen (PSA) test, the digital rectal examination (DRE), the Gleason score and the American Joint Committee on Cancer (AJCC) TNM system, which provides information on the tumor, lymph node involvement and metastasis of a cancer. Imaging tests, such as a PET/CT scan, may also help determine your cancer’s stage.
The four stages of prostate cancer are subdivided into more precise categories, but we generally refer to three groups that indicate how far the cancer has spread:
- Localized: There’s no indication that the cancer has spread beyond the prostate.
- Regional: There’s evidence of cancer cells in nearby lymph nodes or tissue.
- Distant: There’s evidence the cancer has spread to other organs or body parts farther from the prostate.
Almost 90 percent of prostate cancers are diagnosed at the localized or regional stage. The five-year relative survival rate for men diagnosed with prostate cancer at these stages is nearly 100 percent.
Prostate cancer risk assessment
While staging the cancer is based on evidence indicating where the disease is located now, doctors also try to determine the probability that localized or regional cancer has microscopically progressed, or is likely to progress, outside the prostate.
This process is known as a risk assessment or risk stratification. (Distant cancer isn’t assigned a risk category because there’s evidence that it’s metastasized. It may also be referred to as advanced prostate cancer.)
Information obtained from biopsy results, PSA tests, your Gleason score and your TNM score factor into your risk assessment. Risk groups are categorized as very low, low, favorable intermediate, unfavorable intermediate, high and very high risk.
Advanced genomic testing is another tool that may help predict how aggressive your cancer is if it identifies known abnormalities that may be driving the growth of your cancer. Genomic testing may also reveal additional treatment options if you have advanced metastatic disease.
Treatment guidelines for prostate cancer
The National Comprehensive Cancer Network Guidelines detail appropriate prostate cancer treatment options according to a patient's risk group and life expectancy (a factor of the patient’s age and general health).
For patients with very low-risk, low-risk and some favorable intermediate-risk disease, the guidelines recommend active surveillance, surgery or radiation therapy. Different treatment options, or combinations of treatments, are recommended for some intermediate-risk and for high-risk patients. These patients may receive hormone therapy in addition to surgery and/or radiation, for example.
What the research shows about radiation vs. surgery
The ProtecT trial was a 10-year, randomized clinical study designed to compare radical prostatectomy, external-beam radiotherapy and active surveillance for the treatment of localized prostate cancer.
The results, published in 2016, showed that the rate of disease progression among men assigned to radiotherapy or radical prostatectomy was less than half the rate among men assigned to active monitoring. However, there was no significant difference in survival at the median 10-year follow-up for radiation therapy, surgery or active surveillance.
If you’re interested in directly comparing treatment outcomes by treatment method and risk group (low, intermediate or high), the Prostate Cancer Free Foundation provides an interactive graph on its website with information from data obtained from over 129,000 prostate cancer patients over a 15-year period.
As discussed earlier in the sections on the side effects of radiation therapy and surgery, the researchers conducting the ProtecT trial also looked at side effects and quality-of-life issues and found that the three major side effects of these two treatment options that affect quality of life after prostate cancer treatment are urinary incontinence, sexual dysfunction and bowel health.
The trial found that urinary leakage and erectile dysfunction were more common after surgery than after radiation therapy. Gastrointestinal bowel problems were more common after radiation therapy.
Are surgery and radiation therapy ever used together?
In some cases, your care team may use both surgery and radiation therapy as part of your prostate cancer treatment plan. Typically, radiation therapy is delivered after surgery to target remaining cancer cells or that came back. However, in some situations, doctors may recommend radiation therapy first to kill cancer cells in tissues near the prostate gland before performing the prostatectomy.
Get a second (or even a third) opinion
Before making a treatment decision, seek several opinions. If possible, consult with a radiation oncologist and a urologic oncologist. Each field of specialty has its own area of expertise.Together, they may provide a more accurate assessment of your particular condition, which will help you make a more informed decision about the best prostate cancer treatment for you.
Your specific health conditions could mean that one choice may be better for you than the other. For example, if you have urinary obstructive symptoms that don’t respond to medical management, surgery might be a better option for you. On the other hand, if you have another health condition, such as a cardiac condition that makes surgery riskier for you, radiation therapy may be the better choice.
When you meet with doctors, ask for statistics and the risk of possible side effects for their recommendations. And, ask about what’s important to you. For example, if you have inflammatory bowel disease, you might not want radiation therapy, which is known to cause a higher number of bowel problems. If you’re very concerned about urinary leakage, you might choose radiation therapy over surgery.
You may have to seek appointments with these doctors individually. Ask if they’ll consult with one another about your case.
An alternative is to seek an opinion from a multidisciplinary group of oncologists and cancer care experts who will offer an unbiased, expert opinion on your case. This is what we do for our patients at CTCA.
How we approach prostate cancer treatment at City of Hope

When you come to City of Hope for a diagnostic consultation or second opinion, your case is reviewed by a multidisciplinary team of genitourinary cancer experts before you arrive for your first appointment. This care team may include a medical oncologist, a urologist or urologic oncologist and a radiation oncologist.
If we determine you need additional diagnostic evaluations, such as imaging or genomic testing, we schedule those procedures for you before your arrival.
We’ll also schedule appointments for you with our integrative care providers, who work to prevent and manage side effects of cancer and its treatment.
Together, we develop a treatment plan that’s based on your unique needs—usually within two to three days. Our goal is to give you and your caregivers a clear understanding of your options to empower you to make an informed decision about your care.
At City of Hope, we strive to treat our patients as we would want our own loved ones to be treated: with compassion, dignity and respect.
Making your decision
Most prostate cancer patients enjoy a good quality of life after treatment. If you feel pressure to make an immediate decision, take a step back. Most men with early-stage prostate cancer have time (within reason) for a second opinion and to think through their options.
Research bears out that there is no “right” decision when it comes to deciding between radiation or surgery for localized prostate cancer. There’s only the decision that’s right for you.
If you’d like to schedule a second opinion with our multidisciplinary team of prostate cancer experts, call us or chat online with a member of our team to schedule an appointment.
Want to learn more about prostate cancer?


