When a celebrity’s cancer diagnosis becomes public, it’s often about more than generating publicity. After all, cancer is serious business, and no amount of fanfare or TV facetime will have any effect on the celebrity’s recovery or outcome. Often, a star’s diagnosis shines a light on specific aspects of cancer screening, treatment or other issues, whether they choose to go public with it or not.
When Chadwick Boseman died of cancer at the age of 43, for instance, it brought awareness to the alarming rise in colorectal cancer cases among young adults. When her first husband Jay Monahan died of colorectal cancer in 1998, journalist and former Today host Katie Couric went public with his diagnosis, in part to encourage people to get screened. In fact, Couric chronicled her colonoscopy on television as part of her campaign.
Now, it’s Couric who’s been diagnosed with cancer. She went public this week with her breast cancer diagnosis and opened up about the details of her treatment and the importance of breast cancer screening.
“Why am I telling you all this?” she wrote on her website. “Well, since I’m the ‘Screen Queen’ of colon cancer, it seemed odd to not use this as another teachable moment that could save someone’s life.”
In this article, we’ll explore these six things we can learn about Couric’s breast cancer diagnosis:
- She delayed her mammogram because of the pandemic.
- She was screened with a 3D mammogram.
- Her dense breasts required additional testing.
- Her treatment and diagnosis included a sentinel lymph node biopsy.
- She was diagnosed with stage 1 breast cancer.
- She chose a lumpectomy instead of a mastectomy.
If you’re interested in undergoing breast cancer screening, or if you’ve been diagnosed with breast cancer and want a second opinion on your diagnosis and treatment plan, call us or chat online with a member of our team.
She delayed her mammogram because of the pandemic
When she was told she was due for a mammogram, Couric told her doctor she had just gotten one. Since her first husband’s death, Couric says, she’s been hypervigilant about her health. But her doctor revealed she had skipped her annual breast cancer screening in 2021.
“How could that be?” she said. “Had the pandemic given me a skewed sense of time?”
Couric wasn’t alone. Since early 2020, when the COVID-19 pandemic forced lockdowns and strained hospital resources, the numbers of cancer screenings plummeted. For instance, a 2022 study of the Veterans Affairs health care system, which accounts for 3 percent of the nation’s cancer diagnoses, revealed screenings in 2019-20 declined:
- 49 percent for low-dose CT scans for lung cancer
- 12 percent for mammograms for breast cancer
- 55 percent for colonoscopies for colorectal cancer
Other studies revealed similar results, prompting concerns of an impending wave of new and advanced-stage cancer diagnoses in the near future.
“How delays in cancer screenings actually impact ultimate outcomes is uncertain,” says Maurie Markman, MD, President of Medicine & Science at CTCA®. “However, in the presence of early symptoms, it’s possible that a delay could lead to a worsening of the symptoms, negatively impact quality of life, lead to the necessity of more aggressive surgery, and result in a more advanced stage of disease.”
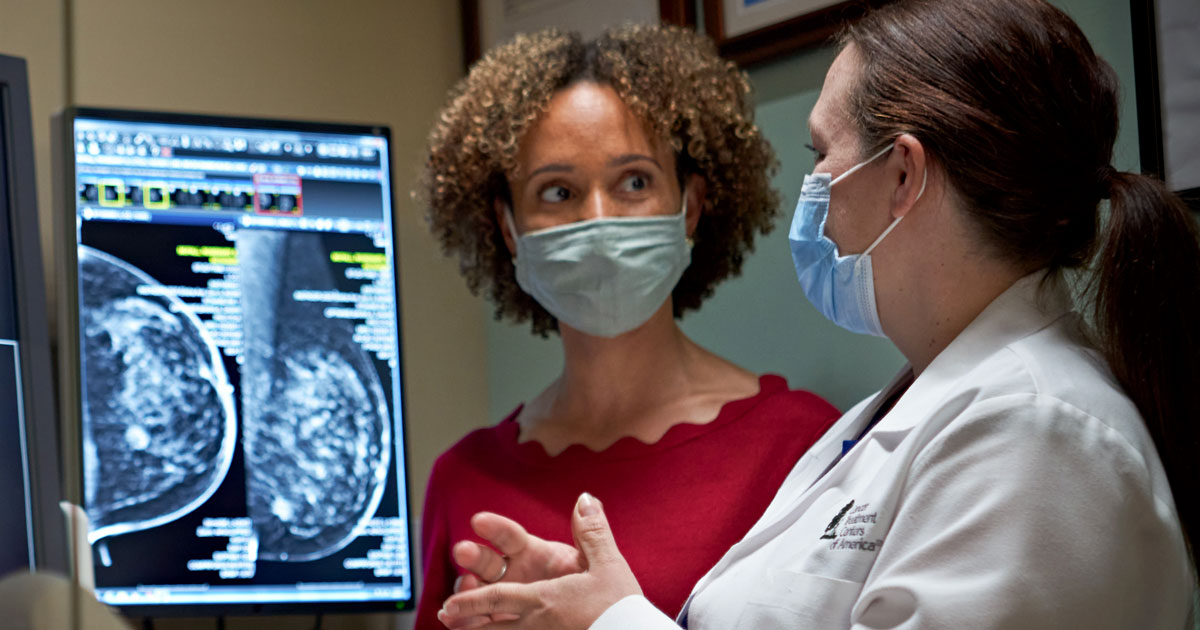
She was screened with a 3D mammogram
Couric received a 3D mammogram, also called digital breast tomosynthesis (DBT), which is considered a major advancement in breast cancer detection. DBT doesn’t exactly produce a 3D image of the breast, but it captures multiple images from various angles to provide a more complete image.
“Digital tomosynthesis excels at what’s most important in mammography,” CTCA Atlanta Radiologist Henry Krebs, MD, wrote in a CancerCenter360® blog. “It’s sensitive enough to find an abnormality and specific enough to separate the abnormality from the overlying tissues, allowing us to see subtle masses and architectural distortion often found with early-stage cancer.”
Dr. Krebs strongly recommends women undergo regular screenings for breast cancer and talk to their doctor about the benefits of DBT mammograms.
“Wherever you decide to get your mammography screenings, the most important takeaway is to get them regularly, and to pay attention to abnormal changes in your breast,” he wrote. “We’ve come a long way in the diagnosis and treatment of breast cancer, and early detection—thanks in large part to advances in mammography—has been key.”

Her dense breasts required additional testing
In her article, Couric revealed she often gets additional screening because she has dense breasts. So, after her mammogram, she underwent a breast ultrasound, which revealed an anomaly. At first, she and her doctors speculated it may have been a scar from Couric’s breast reduction surgery. But a biopsy revealed it was cancer.
It's important for women to talk to their doctor about breast density because it may determine whether additional screening and vigilance are required.
“Women who have more dense breasts have a slightly increased risk of breast cancer,” says Dennis Citrin, MD, Medical Oncologist at CTCA Chicago. “It’s important to find out whether a woman has dense breasts to better understand her breast cancer risk and how sensitive the mammogram will be.”
In some states, doctors are required to inform patients of their level of breast density as determined by a mammogram. About half of American women have dense breast tissue.
Her diagnosis included a sentinel lymph node biopsy
Lymph nodes are bean-shaped nodules connected by vessels that carry lymph fluid through the body. This network of nodes helps produce immune cells and filter out impurities and infections. They sometimes also carry cancer cells, which may be an indication the cancer has spread elsewhere in the body.
It's common for doctors to identify one or more nearby lymph nodes, so-called sentinel lymph nodes, to examine for cancer cells. These sentinel nodes are identified using an injected dye or radioactive material. A pathologist then examines the node to determine whether cancer cells are present and, if so, to help stage the cancer.
“The pathology came back a few weeks later,” Couric wrote. “Thankfully, my lymph nodes were clean.”
She was diagnosed with stage 1 breast cancer
With the lump removed, margins clean and lymph nodes clear, Couric was diagnosed with stage 1A breast cancer.
As with most cancers, the stage of the disease when it’s diagnosed plays a critical role in the patient’s eventual outcome.
When breast cancer is diagnosed at stage 0 or 1, the five-year survival rate is 99 percent. But when the cancer has metastasized, or spread to distant locations in the body, the survival rate falls to 29 percent.
She chose a lumpectomy instead of a mastectomy
A key decision many breast cancer patients need to make is whether their condition requires a mastectomy or a lumpectomy. What’s the difference?
A mastectomy removes the entire breast, while a double mastectomy removes both breasts. Your doctors may recommend a mastectomy if:
- You’re diagnosed with specific types of breast cancer, including invasive breast cancer or inflammatory breast cancer.
- Cancer is detected in more than one area of the breast.
- You have BRCA1 or BRCA2 gene mutations, which increase the risk of a second cancer.
- You’re a male with breast cancer.
A lumpectomy, also called breast conservation surgery, removes only the cancerous tissue and surrounding margins in the breast.
In Couric’s case, surgeons removed a lump about the size of an olive from her left breast.
After her surgery, she received radiation therapy intended to kill cancer cells that may have been left behind by surgery.
She also was prescribed a targeted therapy medication known as an aromatase inhibitor. These drugs are usually given to post-menopausal breast cancer patients to stop some hormones from turning into estrogen, which can promote the growth breast cancer cells.
Common side effects of aromatase inhibitors include:
- Hot flashes
- Vaginal dryness
- Night sweats
- Joint and muscle pain
Couric shared how fortunate she felt that her breast cancer screening was only delayed by six months.
“Please get your annual mammogram,” she wrote. “I was six months late this time. I shudder to think what might have happened if I had put it off longer.”
If you’re interested in undergoing breast cancer screening with us, or if you’ve been diagnosed with breast cancer and want a second opinion, call us or chat online with a member of our team.