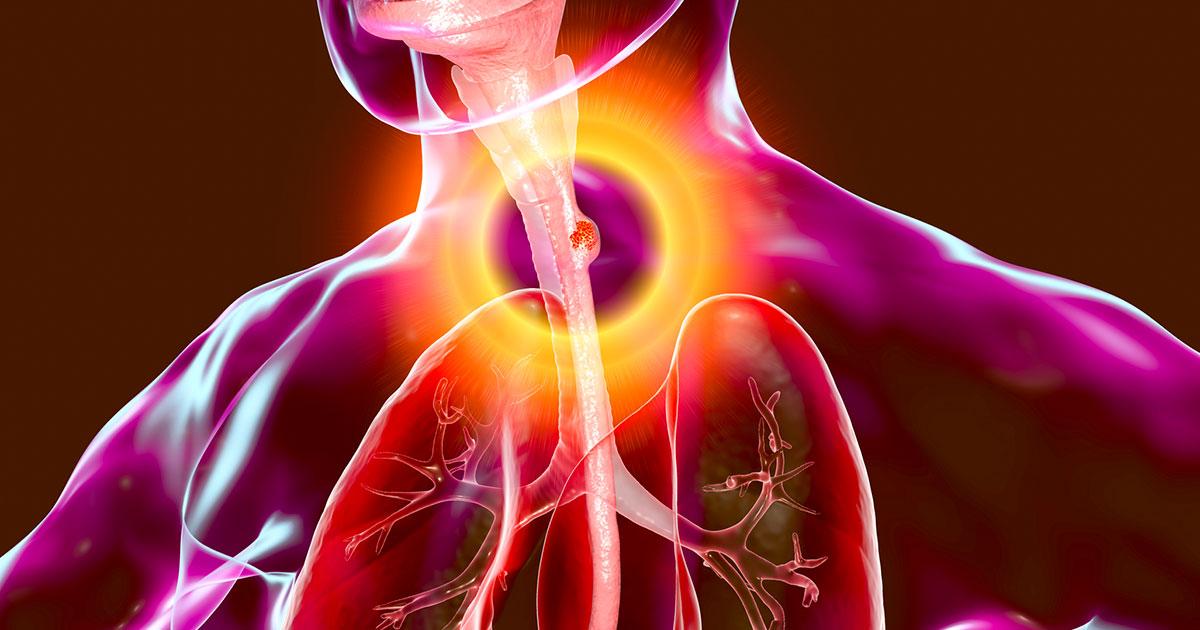
In its early stages, esophageal cancer doesn't often cause symptoms. Patients don't usually start experiencing symptoms such as difficulty swallowing, unintended weight loss, hoarseness and chest pain until the disease has advanced. At this point, it's harder to treat, and the five-year survival rate ranges between 5 and 25 percent, depending on where the cancer has spread.
Catching esophageal cancer earlier, preferably at the precancerous stage, improves patients' long-term survival rates and quality of life. We may even be able to prevent it in certain circumstances.
However, the United States Preventive Services Task Force (USPSTF), an independent body of experts who develop evidence-based recommendations for clinical preventive services in America, does not recommend that the general population get screened for esophageal cancer.
The lack of an official esophageal cancer screening recommendation for an asymptomatic population isn’t necessarily due to the absence of an effective screening procedure, but to its cost, relatively speaking. Unlike colon cancer, for example, which affects over 150,000 Americans every year, about 20,000 people get diagnosed with esophageal cancer per year in the United States. And during a colon cancer screening, we may be able to find and remove pre-cancerous polyps—something not easily done during esophageal cancer screening, meaning that recommending esophageal cancer screening for the general population isn't as cost-effective as a recommendation for colon cancer screening.
But lack of an official recommended screening process doesn't mean we can't identify and screen individuals at high risk of esophageal cancer. If you're one of these high-risk individuals, esophageal cancer screening may help reduce your risk or it may allow you to get a diagnosis when the cancer is more easily treatable.
To help you identify whether you should get screened for the disease, this article covers:
- Risk factors for esophageal cancer
- Benefits of esophageal cancer screening
- Diagnostic screening tools for esophageal cancer
- Steps to take after getting screened for esophageal cancer
If you have questions about esophageal cancer screening or esophageal cancer treatment at Cancer Treatment Centers of America® (CTCA), call us or chat online with a member of our team.
Risk factors for esophageal cancer
Even though the USPSTF doesn't recommend that the general population get screened for esophageal cancer, we know that certain individuals with risk factors for the disease could benefit from screening. These risk factors include:
- Gender: Men are more likely to develop esophageal cancer.
- Race: White men have an increased risk of adenocarcinoma. Black men have a higher risk of squamous cell cancer.
- Obesity: Being overweight increases your risk of developing cancer in general.
- Tobacco use: Smoking and tobacco use increases your risk of esophageal cancer.
- Chronic acid reflux: Over time, acid reflux may cause changes that eventually lead to esophageal cancer.
- Family history: A family history of esophageal cancer and/or Barrett's esophagus is associated with an increased risk of developing the disease.
Individuals who have several of these risk factors should consider getting screened for esophageal cancer. Remember that most patients don't experience symptoms of early-stage esophageal cancer. For those at high risk, screening may allow us to diagnose and treat the disease before it reaches an advanced stage, and it may even help us prevent the cancer when we know the patient suffers from a premalignant condition, such as GERD or Barrett's esophagus.
Get a nutritional plan developed based on your DNA profile.
What is GERD?
A common misconception among patients is that acid reflux (heartburn) is harmless. While occasional acid reflux may be common, a chronic case of acid reflux, otherwise known as GERD, may put you at risk of developing esophageal cancer. By chronic, we mean having acid reflux more than three times a week for more than five years.
While GERD increases your risk of developing esophageal cancer, it doesn’t always lead to it. In fact, the chances of that happening are quite low. While around 66 million Americans have GERD, about 20,000 Americans are diagnosed with esophageal cancer each year. On the other hand, some patients who are diagnosed with esophageal cancer don’t have a history of GERD, so don’t ignore the other warning signs just because you don’t have GERD.
Be aware that if you've suffered from chronic acid reflux and it suddenly goes away without a significant lifestyle change on your part, this warrants a trip to the gastroenterologist. It may be an indication that you’ve developed a condition known as Barrett's esophagus, a precursor to esophageal cancer.
What is Barrett's esophagus?
Barrett's esophagus is a precancerous condition where the lining of the esophagus changes in nature and color as a result of prolonged, chronic exposure to acid reflux. The tissue of the esophagus changes to try to protect itself from the negative effects of acid reflux, and the condition is usually evidenced by a change in the color and texture of the inner lining.
You can think of Barrett's esophagus as the esophageal equivalent of sun tanning. When you expose your skin to sunlight for long periods of time, it adapts, turning a darker color to try to protect itself from the negative effects of sunlight.
The problem is that, just like an overexposure to sunlight increases the incidence of skin cancer, a change to the inner lining of your esophagus increases your risk of developing esophageal cancer.
The progression from the initial development of Barrett's esophagus to esophageal cancer is defined by four steps:
- Esophageal dysplasia (the equivalent of tanning)
- Low-grade dysplasia (the equivalent of finding a mole on your skin)
- High-grade dysplasia (the equivalent of that mole changing in size, shape or color)
- Esophageal cancer
An upper endoscopy is a simple procedure that can help your physician determine whether you’ve developed Barrett's and are at risk of developing esophageal cancer.
If you’re diagnosed with Barrett's, a procedure called radiofrequency ablation may be an option. This procedure uses high-energy radio waves to destroy pre-cancerous cells. After this procedure, the lining of the esophagus regrows. It's as if you turned back time on your esophagus.
Benefits of esophageal cancer screening
The two types of esophageal cancer are esophageal adenocarcinoma (more common in the United States) and esophageal squamous cell carcinoma (more common in Asian countries). Both types have four stages to their development:
- Very early, when a small cancer can be removed endoscopically
- Early, when a cancer is too advanced to be removed endoscopically, but can be treated with chemotherapy, radiation therapy or surgery
- Advanced, when the cancer can't be completely treated with chemotherapy, radiation therapy or surgery
- Very advanced, when the cancer has already spread (metastasized) and is no longer considered treatable.
When esophageal cancer screening identifies Barrett’s esophagus and/or the presence of precancerous cells, you and your physician may be able to take steps to prevent cancer through lifestyle changes and/or radiofrequency ablation.
Esophageal cancer screening in high-risk individuals also increases the chances of early detection of asymptomatic esophageal cancer. A diagnosis of very early or early esophageal cancer may result in better survival rates and a better quality of life before and after treatment.
The five-year survival rate for patients with esophageal cancer that hasn’t spread beyond the esophagus is 47 percent. When the cancer has spread to surrounding tissues, organs or regional lymph nodes, on the other hand, the five-year survival rate drops to 25 percent. Esophageal cancer that’s metastasized has a 5 percent survival rate.
Diagnostic procedures for esophageal cancer and Barrett's esophagus

An upper endoscopy or endoscopic screening test is the primary diagnostic procedure to screen for and diagnose Barrett’s esophagus and esophageal cancer.
Through an upper endoscopy (EGD), your physician is able to look at the inner lining of the upper digestive tract. If your physician identifies suspicious areas, he or she may then proceed to take samples of the affected tissue, which can then be analyzed (biopsied) to diagnose esophageal cancer.
Other diagnostic procedures for esophageal cancer include:
Cytology: This procedure is similar to an upper endoscopy, but instead of taking samples of the affected tissue through a biopsy, your physician uses a brush to sample cells from along the inner lining of your esophagus. Artificial intelligence then looks for abnormal cells that may indicate the presence of esophageal cancer.
Endo sponge: This small sponge has a string attached to it. The patient swallows it, and when the sponge reaches the stomach, it expands. The physician then pulls it out, scraping the esophagus. This scraping allows the physician to collect samples of the inner linings of the esophagus in an indirect manner, without the sedation required by an endoscopic treatment or procedure.
Chromoendoscopy: This procedure functions much like a regular upper endoscopy, but with an added light filter that highlights certain characteristics of the esophagus, which in turn helps diagnose Barrett's.
Endoscopic mucosal resection: When a physician finds a lump or lesion in the esophagus during an endoscopy, he or she may elect to remove it entirely through an endoscopic mucosal resection, rather than taking a small sample, as in the case of a biopsy.
Steps to take after esophageal cancer screening
If you’ve undergone esophageal cancer screening, your next steps will be determined by the findings, according to your particular situation.
If no evidence of Barrett’s esophagus or esophageal cancer is found but you’re at high risk of esophageal cancer, your doctor may advise another screening in the future.
If you’re diagnosed with Barrett's esophagus, your physician will determine whether you’re a candidate for radiofrequency ablation. A Barrett's esophagus diagnosis may also warrant regular follow-up screenings to monitor the condition's progression.
In either case, your doctor may advise you to consider lifestyle changes to reduce your risk of developing cancer in the future. When it comes to health care, cancer prevention is often the better approach. Many of the risk factors associated with esophageal cancer, such as obesity and smoking, are lifestyle habits we can control and change, especially with the right help. Losing weight or quitting smoking may reduce not only your risk of developing esophageal cancer, but also your risk of developing many types of cancer.
What to do when diagnosed with esophageal cancer
If you’re diagnosed with esophageal cancer, you should have a conversation with your gastroenterologist and/or oncologist to determine what steps to take next and which treatment options may be appropriate for you.
You may also want to consider getting a second opinion. Many patients come to CTCA® for a second opinion because of our patient-centered, integrative approach and comprehensive treatment options.
We only treat cancer at CTCA, so the members of the gastroenterology departments at each of our locations are experienced in all aspects of esophageal cancer diagnosis and treatment. They work with our team of multidisciplinary oncology experts to develop a plan according to your specific needs.
Cancer research through clinical trials continues to yield treatment advances for esophageal cancer, such as a recently approved immunotherapy treatment used in combination with chemotherapy for some cancer patients with metastatic esophageal cancer. HER2 targeted therapy in combination with chemoradiotherapy is yet another example of treatment advances being made in oncology.
At CTCA, we know the statistics surrounding esophageal cancer, but we also know that each patient is more than a number. We strive to provide our patients with advanced treatment options while treating them with the dignity and respect they deserve.
If you’d like to talk with someone about esophageal cancer screening or esophageal cancer treatment at CTCA, call us or chat online with a member of our team.