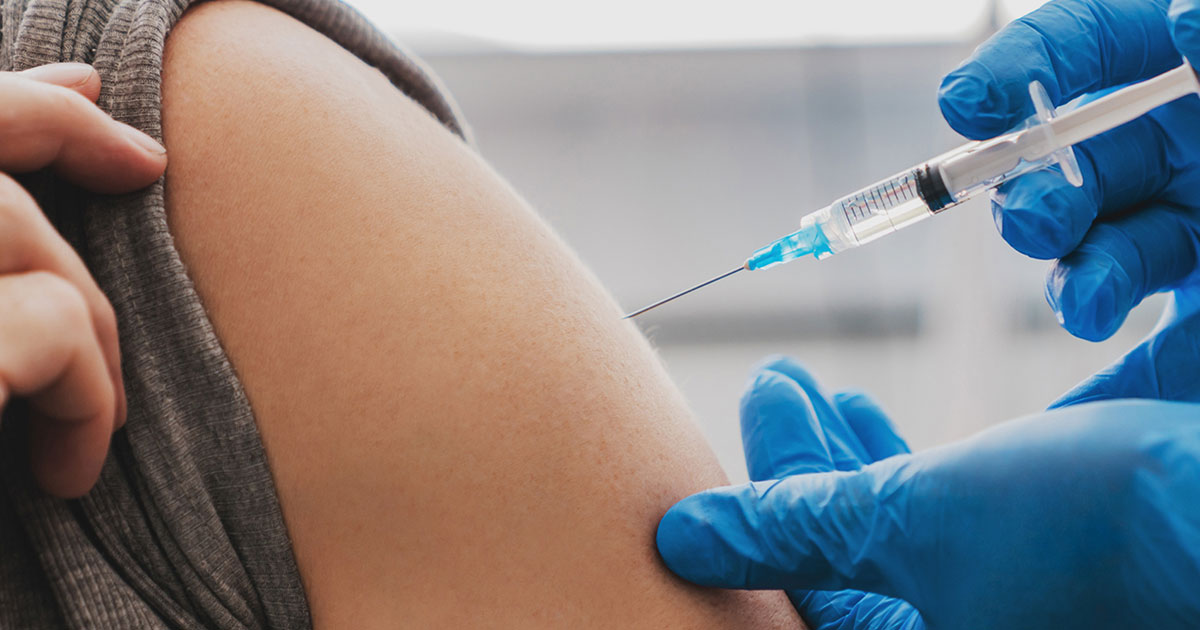
Efforts to end the coronavirus pandemic received a shot in the arm in December when the U.S. Food and Drug Administration (FDA) gave emergency use authorization to two COVID-19 vaccines. The speed at which pharmaceutical companies developed the vaccines is the latest medical marvel in the lifesaving history of inoculations, which help ward off some of the deadliest and most debilitating diseases humanity has faced.
Vaccines have eradicated smallpox, nearly eliminated polio and, until recently, ended measles in the United States. Annual flu shots greatly reduce the risk of influenza symptoms for people who receive the immunizations. Some vaccines are even able to help prevent or treat some forms of cancer.
“However they are formulated or delivered, vaccines will remain the most effective tool we possess for preventing disease and improving public health in the future,” the U.S. Centers for Disease Control and Prevention (CDC) says on its website.
That’s why public health officials are encouraging everyone to be vaccinated against COVID-19, unless they have an underlying medical condition such as an allergy to a vaccine ingredient. Because many cancer patients have compromised immune systems, the COVID-19 and other vaccines offer protection against diseases that may have debilitating effects.
“They should not miss the opportunity of this great way of preventing infection,” says Mashiul Chowdhury, MD, Chief of Infectious Disease at Cancer Treatment Centers of America® (CTCA), Philadelphia.
A vaccine works by introducing a small amount of weakened or mutated disease cells into the body. An immunization shot does not have enough disease cells to make a patient sick, but it has enough to help the body build antibodies that recognize and fight off a disease. A vaccine may help the body know how to prevent certain diseases for an entire lifetime, or the patient may need a booster shot—or “reminder”—years later to keep the disease away.
What do cancer patients need to know about COVID-19 vaccines?
History of vaccines
It has been more than 300 years since British doctor Edward Jenner administered the first smallpox vaccine in 1796. Dr. Jenner discovered that a small amount of a related disease, cowpox, injected into the human body could protect against the more deadly smallpox. Other scientists have built on that approach over the centuries, developing more than 20 vaccines that protect against some of the deadliest diseases, from rabies to cholera. Another couple dozen vaccines are in development to treat other diseases like malaria or the zika virus.
Developing a vaccine isn’t a cure in itself until it gets administered to the people who need it. It took almost 200 years for smallpox to be erased from the globe. The disease was so deadly, it killed up to 300 million people worldwide in the final hundred years before its eradication in 1977.
Polio isn’t nearly as lethal, but in the early 20th century, it was greatly feared as it paralyzed hundreds of thousands of children each year. Even Franklin Delano Roosevelt, the president who led the country out of the Great Depression and through World War II, was not immune. He came down with polio in 1921, when he was 39. Three decades later, in 1953, Jonas Salk developed a vaccine for the disease. Now cases of polio are rare.
Fast forward to today, where standard medical care for infants and young children includes two separate doses of the vaccine for measles, mumps and rubella (MMR). Some parents, misinformed about the vaccine’s safety, refuse to have their children immunized. That reluctance has led to a resurgence of measles, a disease the World Health Organization declared eliminated in the United States in 2000. About 207,000 people worldwide died from measles in 2019, the largest number in 23 years.
Fighting misinformation will be a major challenge for officials trying to achieve widespread immunization from the COVID-19 virus. Since COVID-19 vaccines became available, political leaders have rolled up their sleeves in public to be inoculated in a show of force to inspire confidence in the safety of the vaccines.
The two COVID-19 vaccines now in use in the United States, developed by Pfizer and Moderna, require two shots spaced 21 and 28 days apart, respectively. A third COVID-19 vaccine, by AstraZeneca, is approved for use in Great Britain and by April may be considered for approval in the United States.
Vaccines and cancer
Vaccines have immunized people against many diseases, but a single vaccine used to prevent cancer remains elusive. The variety of forms cancer takes increases the difficulty of finding an inoculation that would work for all.
Vaccine development also takes time. While the current COVID-19 vaccines were developed in less than a year, there is still no HIV vaccine more than 30 years after the deadly AIDS disease spread wildly in the 1980s. Medical professionals have come up with treatments and preventative measures for AIDS, but not a preventative vaccine. A vaccine that prevents all cancers is even more challenging—if it can be done at all.
"Biologically impossible," says Maurie Markman, MD, President of Medicine & Science at CTCA®. "There can't be a vaccine for cancer because cancer isn't a single entity. It's thousands of different conditions."
That doesn’t mean vaccinations are completely ineffective against cancer or of no use to cancer patients. Some vaccines in limited circumstances are being used to prevent or treat cancers. They include:
- Human papilloma virus (HPV) vaccine, which targets potent strains of sexually transmitted HPV to prevent the majority of cervical, throat, anal and head and neck cancers, among others
- Hepatitis B vaccine, which was developed to help prevent some forms of liver cancer
- Bacillus Calmette–Guérin (BCG) vaccine, which was developed for tuberculosis and has since been approved to treat bladder cancer
- Sipuleucel-T (Provenge®) vaccine, an immunotherapy treatment for prostate cancer, specifically for advanced disease that is hormone resistant and has spread beyond the prostate
- Talimogene laherparepvec (T-VEC) vaccine, which uses a herpes virus altered to produce cytokine, to help treat advanced melanoma skin cancer
Vaccines also play a role in cancer care, protecting the weakened immune systems of cancer patients and improving their ability to withstand the disease and its treatments. Some treatments, such as chemotherapy and bone marrow or stem cell transplants, may severely compromise a patient's immune response to infection. It’s important for cancer patients—and their caregivers and family members who could pass a disease onto them—to receive vaccines for the flu and other preventable illnesses. Those protections improve the chances a cancer patient won’t contract those diseases and further weaken his or her ability to recover from cancer.
Patients who receive bone marrow or stem cell transplants may also need boosters or new vaccinations at some point after treatment, because such transplants often reverse the immunization effect of previous vaccines. Patients’ weakened immune systems may also make vaccines less effective during treatment.
Spreading the word about a vaccine’s effectiveness is a major component of any immunization program. Some have had a harder time gaining acceptance than others. For instance, despite overwhelming evidence that shows the HPV vaccine may prevent cancer, the number of girls and young adult women getting the immunization is still very low. Even fewer boys and young men are getting the vaccine, contributing to the rate of HPV-related head and neck cancers in men to surpass that of cervical cancer in women.
Learn more about vaccines and cancer.
Vaccine precautions for cancer patients
Despite the benefits vaccines may offer, cancer patients should talk to their oncologists or health care providers before receiving any immunization. That’s especially true for recently diagnosed patients or those in active treatment. To be effective, some vaccines need a healthy immune system capable of launching a robust attack against a virus.
“If they get a vaccine, generally we wait a week or two before we start active chemotherapy. If they’re already on active chemotherapy, they should wait until the active chemotherapy is complete before they get the vaccine,” Chowdhury says.
Cancer patients also need to avoid live vaccines, those that use live viruses to inoculate against disease. Many vaccines introduce a harmless form of a virus into a person’s body to educate the immune system on what it needs to attack. Vaccines that use live viruses may cause serious side effects for cancer patients, many of whom have weakened immune systems. Cancer patients should also avoid contact with people who have recently received a live vaccine.
“They can actually develop a similar infection by getting the vaccine,” Chowdhury says of the increased risk.
The MMR and yellow fever vaccines both use a live virus. The shingles virus, though related to measles, no longer uses a live virus, making the recombinant zoster vaccine (Shingrix®) suitable for cancer patients, Chowdhury says.
The flu vaccine is not a live virus and cannot give you the flu. According to the CDC, the only people who should avoid the flu shot are those who have had a severe allergic reaction to it in the past. The pneumococcal vaccine, which protects against pneumonia, is recommended every five to six years for individuals ages 65 and older, patients with certain health conditions and all cancer patients.
“You don’t want to have another disease to make your journey complicated and divert you from getting the chemotherapy and the radiation therapy you need,” Chowdhury says. “If someone’s getting admitted to the hospital with pneumonia today, or complications of influenza, we know this patient won’t be able to get the chemotherapy or radiation therapy until they recover from the severe infection or severe sepsis.”
Learn more about COVID-19 vaccine side effects.
Cancer and COVID-19 vaccinations
The new Pfizer and Moderna vaccines both rely on messenger ribonucleic acid (mRNA) to send instructions to cells to produce defenses against the coronavirus that causes COVID-19. Messenger RNA is one of several forms of RNA, the workforce behind deoxyribonucleic acid (DNA). DNA uses RNA to send instructions to cells to perform different tasks.
Because these vaccines use mRNA and not a live virus, they may be better suited for cancer patients. In fact, several pharmaceutical companies are conducting cancer research through clinical trials of other mRNA vaccines they hope may be able to treat a variety of cancers, including melanoma, esophageal cancer and metastatic disease.
“The messenger RNA technology started with the idea of making some treatment strategy or vaccine strategy for cancer,” Chowdhury says. “This research has been going on for a while. It hasn’t stopped.”
There are still unknowns about the COVID-19 vaccines. While Chowdhury says he is comfortable recommending the vaccines to cancer patients, he says the clinical trials intentionally did not include immuno-compromised individuals.
“All these things I’m saying are from my personal experience and opinion, but there’s no real guidelines from the CDC on what to do with cancer patients and the vaccine,” Chowdhury says. Doctors are awaiting more input from the Advisory Committee on Vaccination Practices, a group of U.S. medical and public health experts that develops recommendations on how to use vaccines, he says.
Other unanswered questions about the approved COVID-19 vaccines include:
- How long will the immunity last?
- Is a vaccinated person still able to transmit the virus?
- How will I know my vaccine works for me?
Because of these unknowns, health experts recommend people continue to wear masks and practice social distancing even if they have been vaccinated. Chowdhury says those questions shouldn’t stop cancer patients from receiving the vaccine to prevent COVID-19 infection because they are at higher risk of severe illness.
“I think vaccination for cancer patients is extremely important, because this particular category of patients is in the high risk of a bad outcome from COVID-19,” he says. “We need to protect our cancer patients as much as we can.”
Get answers to questions about COVID-19 vaccines for cancer patients.