Radiation is often a critical component of cancer care, whether it’s used for diagnosing disease or treating it. But the use of the word radiation in various forms may cause confusion for some cancer patients.
Patients often have several doctors and clinicians on their care team with similar titles starting with “rad” — from radiation oncologists to radiologists and radiation therapists to radiologic technologists to radiology technician. So, the confusion is no surprise.
“A patient may say, ‘I met with my radiology oncologist,’ but as doctors, we’re never offended,” says Kevin King, MD, Assistant Clinical Professor of Radiation Oncology at City of Hope® Outpaitient Care Center in Downtown Chicago. “We understand that there’s a lot going on in their lives when we’re introduced into their care. We all share the common goal of making sure the patient gets the best care possible. That’s what matters.”
Still, clearing up confusion around the different titles may help you feel more comfortable and confident in your treatment. That’s why, in this article, we’ll explore:
- What does a radiologist do?
- What is a radiologic technologist?
- What is a radiation oncologist?
- What is a radiation therapist?
- What is an interventional radiologist?
If you’ve been diagnosed with cancer and are interested in a second opinion on your diagnosis and treatment plan, call us or chat online with a member of our team.
What does a radiologist do?
To begin with, all “rads” work with some form of radiation, but how they use it may vary greatly.
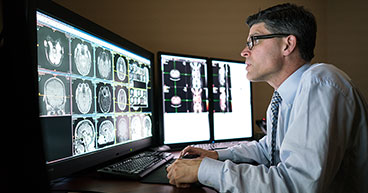
Radiologists primarily work with diagnostics, for example, meaning they use X-rays and other imaging procedures, such as CT (computerized tomography) scans, to take pictures of parts of the body and then interpret what those images mean. Once a radiologist has used images to arrive at a diagnosis, his or her involvement — at least with cancer patients — typically ends.
“Most radiologists have pretty limited patient interactions,” Dr. King says, although some radiologists have specialized training in specific fields, such as mammography, that may increase their engagement with patients. For instance, in addition to reading a patient's mammogram, they may also be responsible for performing biopsies and breast exams.
What is a radiologic technologist?
Both radiologists and radiation oncologists work with larger teams to help them diagnose or treat patients.
Radiologists work with radiologic technologists (sometimes called radiographers), who specialize in taking images for diagnosing injuries and diseases. They then deliver the images to radiologists to interpret.
What is a radiation oncologist?
While radiologists are focused on diagnosing cancer, radiation oncologists are focused on treating it.
“We still use medical imaging,” Dr. King says, “but instead of using it to diagnose something that may be going on, we use it for treatment purposes — to deliver targeted energy to kill cancer cells and shrink tumors.”
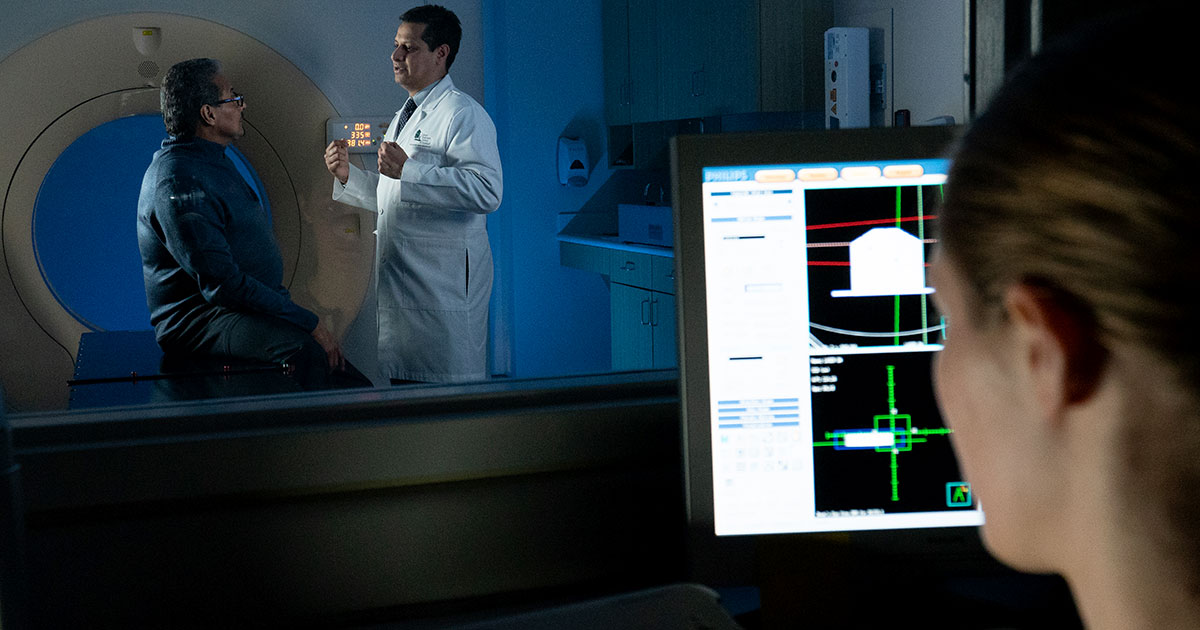
Radiation oncologists use the images a radiologist has already taken and interpreted to determine if radiation therapy is needed. They then meet with the patient to go over the proposed treatment plan.
“We have an ample amount of time to sit down and explain to a patient what’s being done, where their cancer is and what their treatment options are,” Dr. King says. “And then we follow up with them during and after their radiation therapy treatment to see if there are any side effects. So, radiation oncologists commonly have long-lasting relationships with their patients.”
What is a radiation therapist?
Radiation oncologists tend to work with radiation therapists, who — similar to radiologic technologists — are in the room, or a protected adjacent room, with the patient when the radiation is delivered. In such cases, radiation therapists ensure patients are in the proper position to maximize the therapeutic effects of the treatment, which is generally delivered in small doses every day over a period of time, as well as minimize any harm to surrounding tissue.
Though they’re not doctors, radiation therapists are highly trained to operate a variety of sophisticated radiation therapy equipment used in cancer treatment.
A radiation oncologist reviews the daily positioning of patients by radiation therapists and either approves it or suggests changes.
“We may say, ‘I noticed the patient’s tilted a little bit,’ or maybe, ‘I want their bladder just a little bit more full in order to move any organs out of the radiation field so they don’t experience increased toxicity or side effects from the radiation we deliver,’” Dr. King says.
What is an interventional radiologist?
Interventional radiologists are doctors who diagnose and treat a variety of diseases, including cancer, using minimally invasive procedures, typically as an alternative to traditional surgery. For cancer patients, they may use chemoembolization — a procedure that injects chemotherapy medicine into the arteries that feed a tumor — to cut off its blood supply, or radiofrequency ablation — a procedure using heat made by radio waves — to damage cancerous tissue.
“Interventional radiologists are kind of a combination of radiologist and radiation oncologist,” Dr. King says. “They use radiology to perform very specific procedures.”
If your doctor recommends radiation as part of your treatment plan, you should talk to him or her about your options and the length of recommended treatment, Dr. King says.
And don’t worry if you mess up the titles of the “rad” specialists on your healthcare team.
“It wasn’t until about two years ago that my parents stopped telling people their son was a radiologist,” Dr. King says, “so getting the terminology perfect is not a big deal. What is a big deal is making sure you feel safe and comfortable with your treatment plan.”
If you’ve been diagnosed with cancer and are interested in a second opinion on your diagnosis and treatment plan, call us or chat online with a member of our team.