There’s a lot not to like about undergoing chemotherapy and it’s understandable you may be worried about the treatment. But you should be skeptical when worst-case scenarios are talked about as cold hard facts: You’ll lose all your hair; you’ll throw up constantly; you won’t be able to have children.
These side effects are not as common as you might believe.
Yes, chemotherapy is a systemic treatment that carries toxic chemicals throughout your body. It takes its toll as it attacks rapidly growing cancerous cells and healthy cells alike. But medical advancements have made cancer drugs much more tolerable for those who need chemotherapy as part of their cancer treatment regimen.
“Chemotherapy has a very bad rap,” says Dennis Citrin, MD, a Medical Oncologist at City of Hope Chicago. “While the cancer treatment itself has evolved for the better over the past few decades, its public perception hasn’t quite caught up. Educating patients about the facts is such an important piece of what we do every day.”
According to a study published in the June 2019 Lancet Oncology, more than half the new cases of cancer worldwide—excluding non-melanomatous skin cancers—required chemotherapy treatment. Going into the future, the study said the most common cancers treated with chemotherapy will be forms of lung cancer, breast cancer and colorectal cancer.
Because so many cancer patients are likely to have chemotherapy recommended to them, they should understand the truth and the myths regarding the treatment.
This article will cover:
- One chemotherapy drug can treat any cancer type
- Intravenous chemotherapy is the only option
- Chemo sickness affects everyone
- Chemotherapy hair loss affects everyone
- You can’t have kids after chemo
If you’ve been diagnosed with cancer and are interested in a second opinion on your diagnosis and treatment plan, call us or chat online with a member of our team.
Myth: One chemotherapy drug can treat any cancer type
Many people think all types of cancer can be treated with the same chemotherapy drug and that’s simply not the case.
This idea of a single chemotherapy drug may be one of the biggest misconceptions about the treatment. People facing a cancer diagnosis often may not realize that one patient’s chemotherapy regimen may be very different from someone else’s, even if they have a similar cancer.
Reality: Different chemo drugs target different cancers
More than 100 different chemotherapy drugs are used in cancer treatment.
Different drugs target different types of cancer and work in different ways. Some destroy cancer cells, others are used to shrink tumors, while still others are designed to relieve symptoms of advanced cancer. These drugs may be given before, after or in conjunction with other treatments.
In addition, in targeted therapy, a chemotherapeutic agent may be attached to a monoclonal antibody that will bring the cancer-fighting drug directly to the tumor and may have less of a negative impact on healthy cells elsewhere in the body.
Myth: Intravenous chemotherapy is the only option
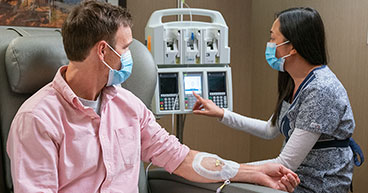
When many people think of chemotherapy treatment, they may envision getting an intravenous (IV) infusion as part of an extended hospital stay. For years, this was the primary way of receiving treatment. The cancer drugs were given through a needle inserted into a vein. The hospital setting may have been preferred because doctors at the time had far less control over the serious side effects chemotherapy may produce.
Reality: Chemotherapy comes in many forms
Today, chemotherapy drugs are often given in an infusion facility at a clinic or hospital and on an outpatient basis.
But it’s possible you may receive your chemotherapy another way. Types of chemotherapy include those listed below.
Oral chemotherapy: You swallow a pill, capsule, or liquid. These drugs may be given daily or on a less-frequent schedule. Oral chemotherapy is usually more convenient because it may be taken at home. But the pills are very toxic and need to be handled with care.
Injected chemotherapy: You get a shot of a chemotherapy drug. There’s no specific site for an injection; it will differ depending on your cancer and the drug being used. It may be injected into muscle or under the skin, into an arm or leg, or even the abdomen or some other body area.
Topical chemotherapy: You receive a cream that is applied to an area of skin. You may pick up your prescription at a pharmacy and apply it at home.
Myth: Chemo sickness affects everyone
Just 25 years ago, chemotherapy was associated with intense nausea and vomiting, and that reputation was well deserved. But, as with so many cancer treatments, advances have been made since then to improve the effectiveness of cancer drugs and reduce their side effects.
How intense your reaction will depend on the type of cancer drug being used, how high a dose you receive, the way it is administered, how frequently it is given and the functioning of your own body. Your doctor may adjust levels depending on how you are affected.
Reality: Chemotherapy side effects may not be as debilitating as they once were
Today, many chemotherapy drugs are designed in part to prevent nausea and vomiting, or to reduce their severity. Research has informed oncologists about optimal dosage levels and recommended frequencies for receiving the different chemotherapy regimens. This helps the doctors determine a course of treatment to lessen side effects as much as possible while also providing a sufficient level of cancer-fighting drugs.
“We often tell our patients that if they’re throwing up all day, we’re not doing our job,” Dr. Citrin says.
A wider variety of medicines are also available that may help alleviate or reduce nausea or vomiting during treatment. Your doctors has information, such as guidelines put out by the American Society of Clinical Oncology, to show which medicines work best at preventing nausea based on the chemotherapy drugs you have been prescribed.
In many cases, you begin taking the anti-nausea, anti-vomiting medications before you start your chemotherapy treatment. That way, such side effects can be prevented before they start, the American Cancer Society says.
Myth: Chemotherapy hair loss affects everyone
One distressing concern for people facing chemotherapy is that they may lose all their hair, even eyelashes and eyebrows, as well as on other parts of their bodies. Because chemotherapy is designed to attack rapidly growing cells, some chemotherapy drugs weaken or damage hair follicles, causing hair to fall out.
But hair loss isn’t inevitable.
Reality: Chemotherapy hair loss depends on many factors
Some drugs are more likely to cause hair loss than others, and the risk varies widely. Hair that falls out due to chemotherapy usually does so two to three weeks after the first treatment
While there is no known drug that can eliminate hair loss from chemotherapy, wearing a cooling cap is one possibility that may help. By cooling the scalp, the caps may cause blood vessels to constrict, thus limiting how much of the chemotherapy drug reaches hair follicles, according to the National Institutes of Health.
Myth: You can't have kids after chemo
For many women, menstruation stops during chemotherapy treatment. However, if a woman is in her 20s, 30s or even early 40s, she will likely menstruate again after treatment ends. “It really depends on the age of the patient,” Dr. Citrin says, “but in most cases, a woman’s periods will return after treatment ends unless she’s close to menopause or already through it.”
Patients who are pregnant when diagnosed with cancer may be prescribed certain chemotherapy drugs that do not impact the baby, so it’s possible pregnancy may not impede chemotherapy treatment, either.
Reality: Many people have children after chemotherapy
While some chemotherapy treatments may result in infertility, not everyone who receives chemotherapy is unable to have children. And even for those who are more likely to become infertile because of their treatments, options are available before treatment to preserve eggs or sperm for a future conception.
Depending on the chemotherapy, some female cancer patients will be advised to wait six months before trying to become pregnant, to provide a chance for damaged eggs to be released from the body. Other medical professionals suggest waiting two years to five years after treatment to ensure the cancer does not return, which may be more difficult to treat during pregnancy.
Cancer patients also can take steps to account for potential infertility, such as a female patient having eggs harvested for future fertilization, having a male patient place sperm in a sperm bank for future use, or preserving frozen embryos for implanting after treatment is completed.
Because chemotherapy has changed so much over the years, and because it is essential to many cancer patients’ treatment plans, education is vital.
“Until recently, many people thought that if chemotherapy was prescribed, the cancer must be terminal,” Dr. Citrin says, “but that’s far from the case. So, it’s not so much dispelling ‘myths’ as it is helping people learn the facts.”
If you’ve been diagnosed with cancer and are interested in a second opinion on your diagnosis and treatment plan, call us or chat online with a member of our team.