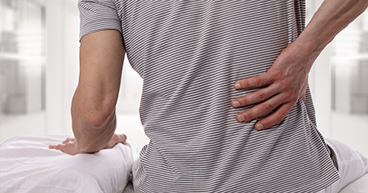
When you have cancer, pain often develops as a side effect of the disease or in response to treatment. But many medications, therapies and techniques are available, and it’s important to speak up about any discomfort you may be feeling—because getting relief is important to your treatment. If pain is under-treated, patients may do worse—they’re not as active, their energy level goes down, they experience increased fatigue and diminished appetite, and they don’t tolerate treatment as well.
It doesn’t have to be that way. Think of controlling cancer-related pain as part of your treatment, and talk candidly with your doctor and health care team so they can try to help you manage your pain.
Five facts
Here are five things you should know about cancer-related pain:
It is different from other chronic pain. Cancer-related pain can stem from many different factors—the tumor pressing on nerves and tissues around it; medical assessments, such as a biopsy or bone marrow test; or chemotherapy, radiation therapy, surgery or other treatments. And unlike chronic pain, the nature of cancer pain can change rapidly. Doctors say it is important to be frequently reassessed so that treatments can be adjusted. Without this, the pain can really debilitate people and it can increase your sensitivity to pain if it’s not controlled.
It’s not enough to say you’re in pain. You need to talk specifically about how you’re feeling and how the pain is affecting you. Start by describing what part of the body hurts, what the pain feels like (burning, shooting, throbbing, or a persistent dull ache, for example), its severity, how frequently it happens, how long it lasts, and how it may be interfering with your activities. If you are also experiencing nausea, vomiting, fatigue, a cough or other side effects, mention those, too.
Every patient needs a personalized pain management plan. It should be based on the type of cancer you have and its stage, your personal sensitivity or tolerance to pain, and how the pain is affecting you. It should also take into account your other medications, your medical history and your personal preferences for pain control.
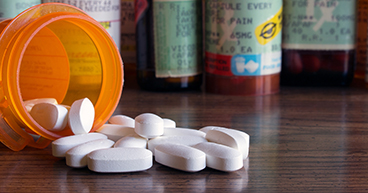
Pain management is improving. Pain management options continue to grow, including opioids, anti-inflammatory drugs, medications for nerve pain, nerve blocks, antidepressants and anticonvulsants. You also may want to consider evidence-based supportive therapies such as acupuncture, massage, meditation, guided imagery and physical therapy to help you manage cancer-related side effects.
Poorly controlled pain can take a toll on your body, mind and spirit. Besides being physically debilitating, unrelenting cancer-related pain can cause you to worry about the future and grieve the loss of your previous day-to-day life. It may also trigger changes in the brain that can exacerbate and accentuate the pain. That’s why you need to act as your own advocate and work with a pain management physician who has experience with cancer patients. Be sure to ask about the different options available.